 |
 |
- Search
| Asian Spine J > Volume 18(3); 2024 > Article |
|
Abstract
Purpose
Overview of Literature
Methods
Results
Conclusions
Notes
Supplementary Materials
Supplement 1.
Supplement 2.
Fig. 1.
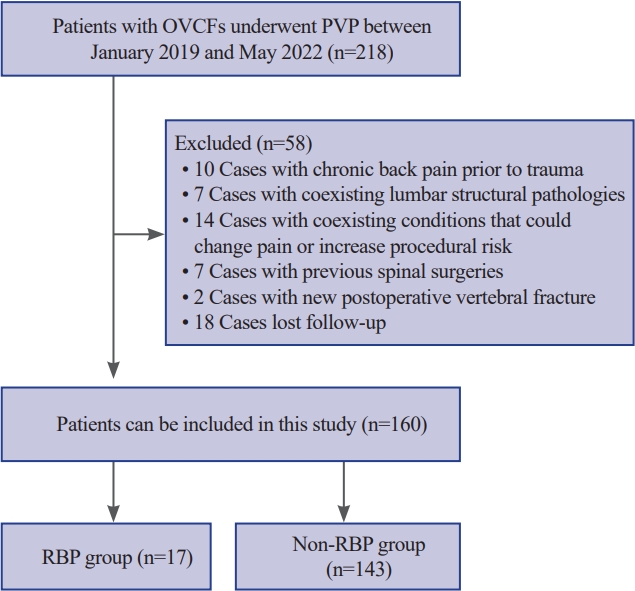
Fig. 2.
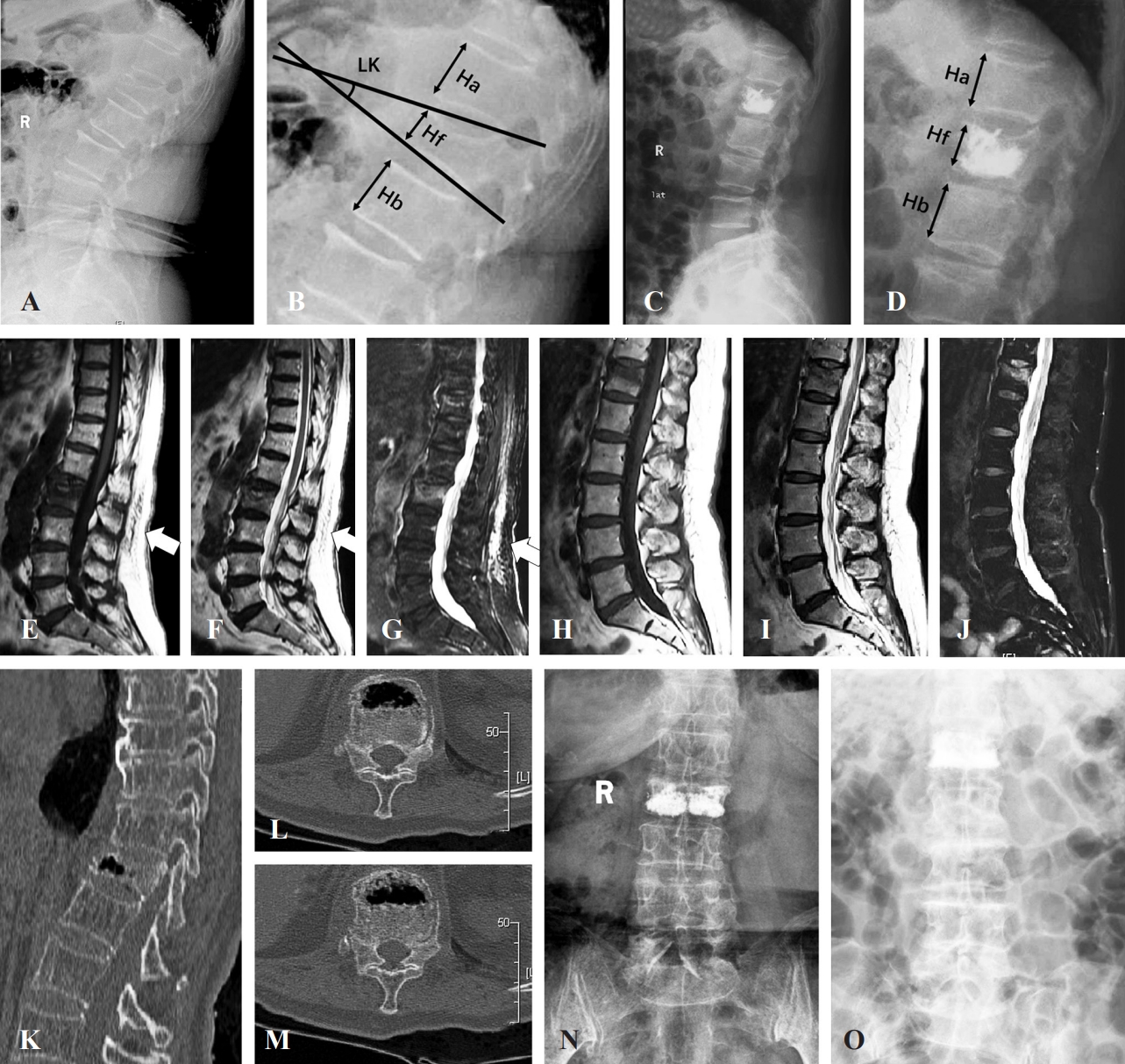
Fig. 3.
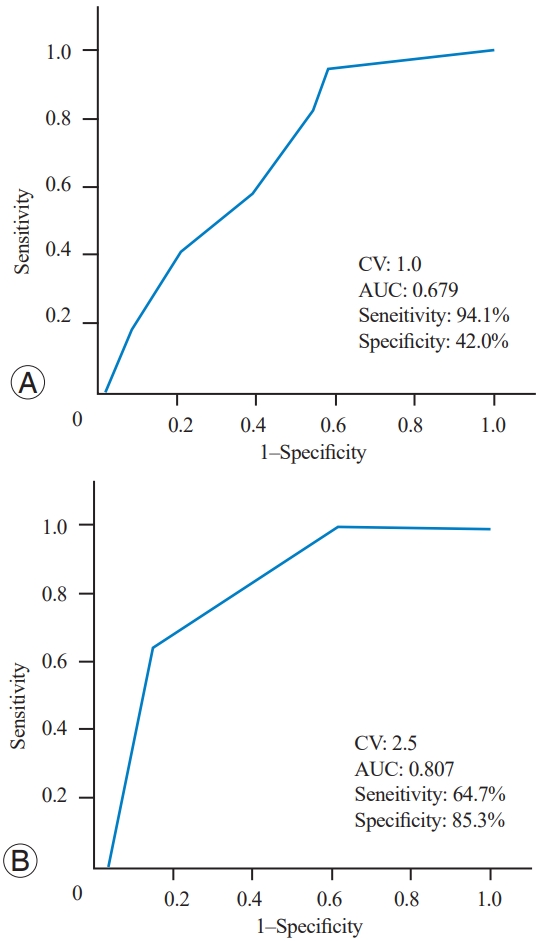
Table 1.
| Characteristic | RBP group | Non-RBP group | Total patients |
|---|---|---|---|
| No. of subjects | 17 | 143 | 160 |
| Age range (yr) | 75.4±7.4 | 75.2±8.0 | 75.2±8.0 |
| Boby mass index (kg/m2) | 24.2±3.3 | 24.0±3.7 | 24.1±3.7 |
| Gender | |||
| Male | 5 | 26 | 31 |
| Female | 12 | 117 | 129 |
| Bone mineral density (T-score) | -3.1±0.7 | -3.4±0.7 | -3.3±0.7 |
| Disease duration (day) | 47.7±35.3a) | 17.1±18.5a) | 20.3±22.8 |
| No. of fracture segments | 1.3±0.6a) | 1.1±0.3a) | 1.1±0.4 |
| Imaging assessments (no./total patient) | |||
| Vertebral height loss (%) | 26.0±11.2 | 23.7±10.7 | 24.0±10.7 |
| Local kyphotic angle (°) | 15.1±7.8 | 15.0±7.6 | 15.0±7.6 |
| Intravertebral vacuum cleft | 8/17a) | 18/143a) | 26/160 |
| Posterior fascia oedema | 10/17a) | 28/143a) | 38/160 |
| Surgical-related factors (no./total patient) | |||
| Operation time (min) | 45.4±11.1 | 41.4±11.2 | 41.8±11.2 |
| Cement volume | 4.5±0.9 | 4.5±0.8 | 4.5±0.8 |
| Vertebral height restoration (%) | 10.4±5.7 | 11.8±5.5 | 11.7±5.5 |
| Cement leakage | 4/17 | 17/143 | 21/160 |
| Separated cement distribution | 3/17 | 15/143 | 18/160 |
| Preoperative pain-related assessments | |||
| VAS scores of LBP at rest | 3.9±1.7a) | 2.4±2.3a) | 2.6±2.3 |
| VAS scores of LBP during movement | 6.9±1.2 | 7.2±2.0 | 7.2±2.0 |
| ODI scores | 61.4±20.5 | 61.7±18.1 | 61.7±18.3 |
| Preoperative dynamic QST assessments | |||
| PPT in local pain area (kg/cm2) | 3.5±1.4b) | 4.0±2.2b) | 4.0±2.2b) |
| PPT in pain-free area (kg/cm2) | 4.0±2.2 | 4.5±2.1 | 4.3±2.1b) |
| CPM in pain-free area (kg/cm2) | 0.2±0.6a),b) | 0.5 ±0.8a) | 0.5±0.8b) |
| TS in pain-free area | 2.6±0.5a),b) | 1.7±0.9a),b) | 1.8±1.0b) |
Values are presented as number or mean±standard deviation.
RBP, residual back pain; VAS, Visual Analog Scale; LBP, low back pain; ODI, Oswestry Disability Index; QST, quantitative sensory testing; PPT, pressure pain threshold; CPM, conditioned pain modulation; TS, temporal summation.
b) Statistically significant differences between patients and healthy subjects. Date of healthy subjects from Nie et al. [13] in 2022.
Table 2.
| Variable | Acute fractures | Subacute fractures | Chronic fractures |
|---|---|---|---|
| No. of subjects | 73 | 73 | 14 |
| Preoperative pain-related assessments (no./total patient) | |||
| Patients with LBP at rest | 40/73a) | 47/73 | 12/14a) |
| Patients with LBP during movement | 73/73 | 73/73 | 14/14 |
| VAS scores of LBP at rest | 2.4±2.4 | 2.7±2.3 | 3.2±1.6 |
| VAS scores of LBP during movement | 7.7±2.0a),b) | 6.9±1.9b) | 6.2±1.2a) |
| ODI scores | 66.1±16.8a),b) | 58.7±18.5b) | 54.5±20.3a) |
| Preoperative dynamic QST assessments | |||
| PPT in local pain area (kg/cm2) | 2.9±1.8a),b),c) | 4.9±2.1b),c) | 4.1±1.6a),c) |
| PPT in pain-free area (kg/cm2) | 4.6±1.9 | 4.2±2.3c) | 3.7±1.4c) |
| CPM in pain-free area (kg/cm2) | 0.5±0.7a) | 0.5±0.8 | 0.1±0.5a),c) |
| TS in pain-free area | 1.5±0.9a),b) | 2.0±1.0b),c) | 2.4±0.9a),c) |
Values are presented as number or mean±standard deviation.
QST, quantitative sensory testing; LBP, low back pain; VAS, Visual Analog Scale; ODI, Oswestry Disability Index; PPT, pressure pain threshold; CPM, conditioned pain modulation; TS, temporal summation.
c) Statistically significant differences between the fracture groups and healthy subjects. Date of healthy subjects from Nie et al. [13] in 2022.
Table 3.
| Variable | RBP patient group | Non-RBP patient group |
|---|---|---|
| No. of subjects | 17 | 143 |
| VAS scores | ||
| 1-Day postop LBP at rest | 2.1±1.4a),b) | 1.1±1.3a),b) |
| 1-Day postop LBP during movements | 5.7±0.8a),b) | 3.2±1.6a),b) |
| 14-Day postop LBP at rest | 2.1±1.3a),b) | 0.9±1.1a),b) |
| 14-Day postop LBP during movements | 4.6±0.9a),b) | 3.0±1.2a),b) |
| 1-Month postop LBP at rest | 1.9±1.3a),b) | 0.4±0.9a),b) |
| 1-Month postop LBP during movements | 3.7±0.7a),b) | 2.6±1.2a),b) |
| 6-Month postop LBP at rest | 1.5±1.4a),b) | 0.1±0.4a),b) |
| 6-Months postop LBP during movements | 3.1±1.0a),b) | 1.2±0.9a),b) |
| ODI scores | ||
| 6-Month postop ODI scores | 22.7±8.6a),b) | 16.8±11.4a),b) |
Table 4.
References
- TOOLS






