|
 |
- Search
| Asian Spine J > Volume 11(1); 2017 > Article |
|
Abstract
Purpose
We evaluated the functional, neurological, and radiological outcome in patients with thoracic and thoracolumbar tuberculosis operated through the transpedicular approach.
Overview of Literature
For surgical treatment of thoracic and thoracolumbar tuberculosis, the anterior approach has been the most popular because it allows direct access to the infected tissue, thereby providing good decompression. However, anterior fixation is not strong, and graft failure and loss of correction are frequent complications. The transpedicular approach allows circumferential decompression of neural elements along with three-column fixation attained via pedicle screws by the same approach.
Methods
A total of 47 patients were diagnosed with tuberculosis of the thoracic or thoracolumbar region from August 2012 to August 2013. Of these, 28 patients had progressive neurological deterioration or increasing back pain despite conservative measures and underwent transpedicular decompression and pedicle screw fixation with posterior fusion. Antituberculosis therapy was given till signs of radiological healing were evident (9ŌĆō16 months). Functional outcome (visual analog scale [VAS] score for back pain), neurological recovery (Frankel grading), and radiological improvement were evaluated preoperatively, immediate postoperatively, and at 3 months, 6 months, and 1 year.
Results
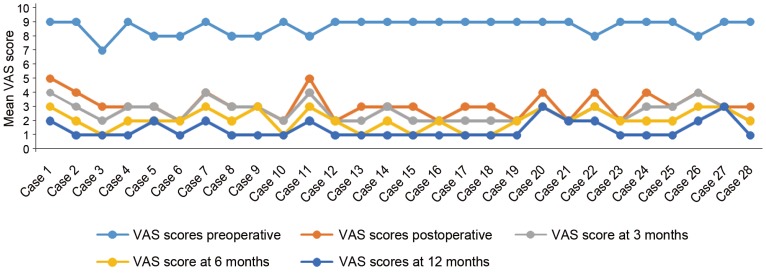
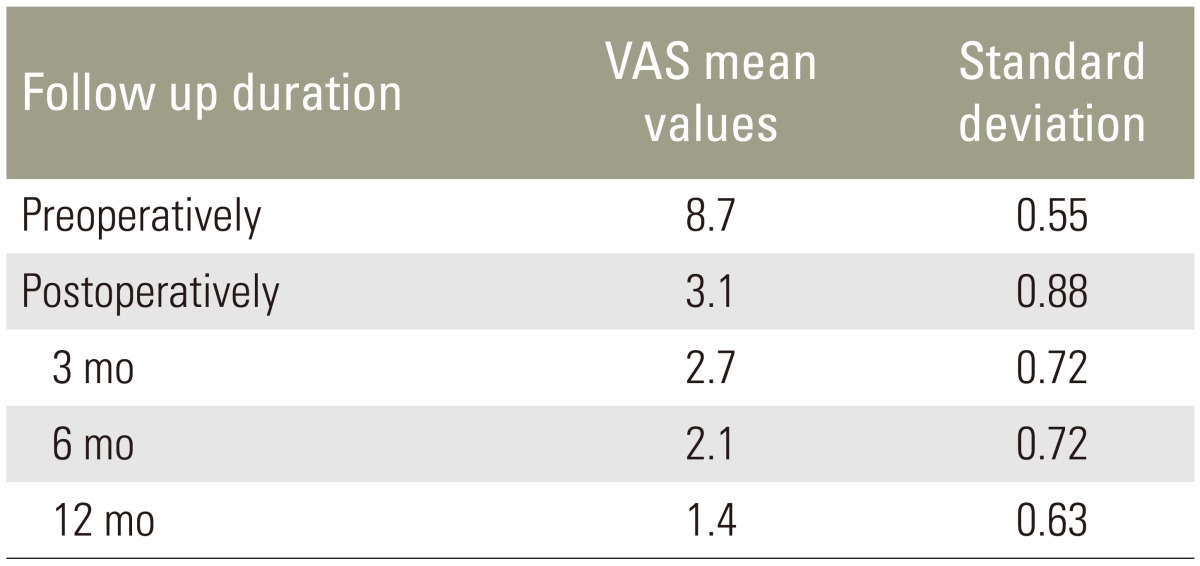
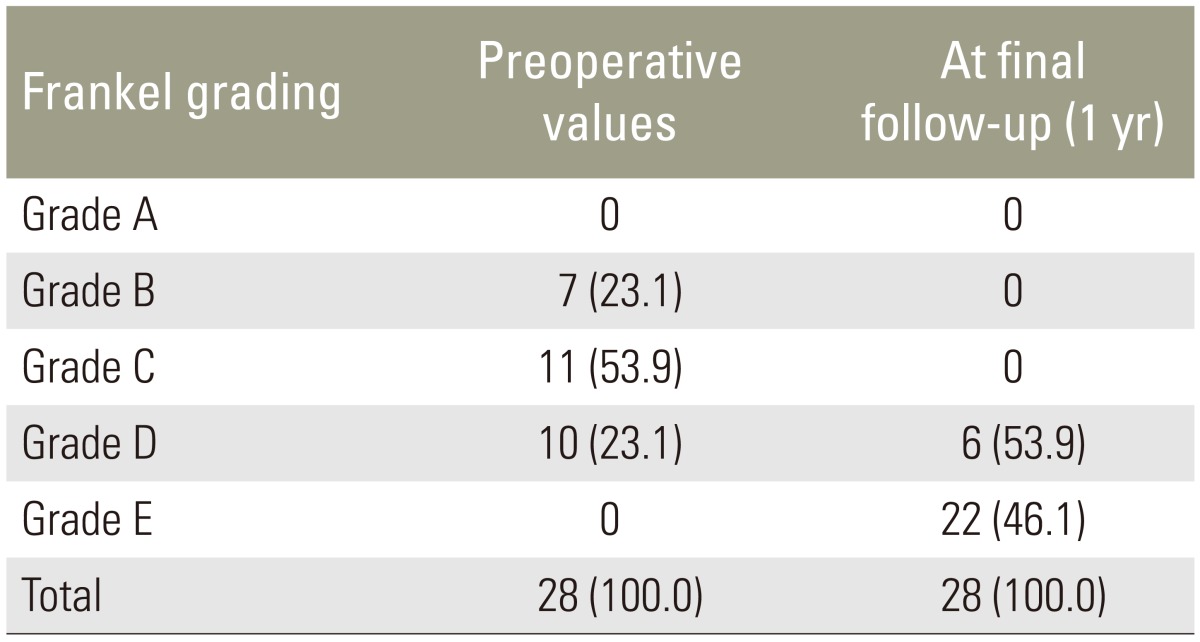
Mean VAS score for back pain improved from 8.7 preoperatively to 1.1 at 1 year follow-up. Frankel grading preoperatively was grade B in 7, grade C in 11, and Grade D in 10 patients, which improved to grade D in 6 and grade E in 22 patients at the last follow-up. Radiological healing was evident in the form of reappearance of trabeculae formation, resolution of pus, fatty marrow replacement, and bony fusion in all patients. Mean correction of segmental kyphosis postoperatively was 10.5┬░. Mean loss of correction at final follow-up was 4.1┬░.
The World Health Organization's Global Tuberculosis Report 2015 ranked tuberculosis alongside human immunodeficiency virus as a leading cause of death worldwide with 1.4 million deaths in 2014 [1]. The spine has been described as the most common site for osseous involvement of tuberculosis, accounting for nearly half of all musculoskeletal tuberculosiscases [2]. The thoracic spine is the most commonly affected region [34]. With radiodiagnostic advancements such as the advent of magnetic resonance imaging (MRI), early detection of disease is now possible, and effective antituberculosis therapy has allowed disease cure in a majority of patients with conservative management alone [5]. However, surgery is indicated in patients with incapacitating back pain or progressive neurological deficits despite commencement of conservative treatment [56].
The aim of surgery in spinal tuberculosis is adequate decompression and stability along with correction of deformity and its maintenance. The anterior approach has been most popular because it allows direct access to the infected tissue, thereby providing good decompression [7]. However, anterior fixation is not strong, and graft failure and loss of correction are frequent complications [6]. A combined approach overcomes stability issues but increases morbidity because of two surgeries (single event or staged). Recently, the extrapleural approach has been popularized because it allows access to the anterior and posterior columns through a single posterior incision [8]. However, it also involves handling of the pleura. All the abovementioned approaches are of high risk in tuberculosis patients as they already have a compromised chest function. The transpedicular approach overcomes all these issues as it allows circumferential decompression of neural elements along with three-column fixation attained via pedicle screws by the same approach [56]. The present study aims to evaluate the results (functional, neurological, and radiological) of the transpedicular approach in operated patients with thoracic and thoracolumbar tuberculosis.
A total of 47 patients with thoracic and thoracolumbar tuberculosis were diagnosed from August 2012 to August 2013. Diagnosis was based on radiological findings (magnetic resonance images) and histopathology reports (samples obtained by computed tomography [CT]-guided biopsy). All patients were started on antituberculosis therapy. Of these, 28 patients developed progressive neurological deterioration or increasing back pain despite conservative measures and underwent transpedicular decompression and pedicle screw fixation with fusion. Our analysis was centered upon these 28 patients managed surgically. There were 13 males and 15 females, and the mean age at the time of surgery was 31.2 years (range, 21ŌĆō58 years). The mean duration of symptoms was 4 months (range, 2ŌĆō7 months). The indication of surgical procedure was intolerable back pain and/or progressive neurological deficits despite ongoing conservative management.
A complete blood count, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), Mantoux test, plain radiographs (anteroposterior and lateral views), and MRI were performed in all patients.
Through a midline posterior approach, laminectomy or laminotomy was performed at the affected levels. Pedicles at the affected level were identified and curetted to reach the anterior and middle columns. The ribs and pleura were not at all exposed. The granulation tissue was removed to decompress the spinal cord. Extensive debridement was avoided. Pedicle screws were fixed two levels above and below. Healthy pedicles of the affected vertebrae were included in fixation. The infected material was sent for histopathological examination and culture sensitivity.
Log roll, side turning, and pelvic lift exercises were started on postoperative day 1, and mobilization with the support of taylor's brace was started as early as possible. Antituberculosis chemotherapy was continued till radiological healing of the lesion was evident. The mean hospital stay was 9 days (range, 7ŌĆō14 days), and suture removal was done on postoperative day 13 in all except one case with superficial infection (day 17).
Functional outcome (visual analog scale [VAS] for back pain) [9], neurological recovery (Frankel Grading) [10], and segmental kyphosis (in plain radiographs) were assessed preoperativelyand postoperativelyat 3, 6, and 12 months following surgery. MRI was done every 4 months postoperatively till signs of radiological healing were evident. Segmental kyphosis was measured as the angle between the caudal and cephalic end plates nearest to the lesion.
Preoperatively, the mean white blood cell count was 8,800 (5,400 to 12,300). The ESR was elevated in 17 cases (60.7%), and the CRP level was elevated in 22 cases (78.6%). The Mantoux test was positive in 12 cases (42.8%), and the histopathological reports demonstrated tubercular osteomyelitis in all the 28 cases with the presence of typical caseating granulomas. However, culture was positive only in 8 (28.6%) cases.
The mean VAS score for back pain improved from 8.7 preoperatively to 1.1 at the final follow-up (1 year) (Table 1, Fig. 1). Frankel grading preoperatively was grade B in 7, grade C in 11, and Grade D in 10 patients, which improved to grade D in 6 and grade E in 22 patients at 1 year (Table 2). Radiological healing was evident in the form of reappearance of trabeculae formation, resolution of pus, fatty marrow replacement, and bony fusion on sequential follow-ups in all cases (Fig. 2). All except one patient healed at 1 year follow-up. One patient had pocket of pus in the psoas muscle and healed at the end of 17 months. The mean correction of segmental kyphosis postoperatively was 10.5┬░ (range, 5┬░ŌĆō17┬░). The mean loss of correction at the final follow-up was 4.1┬░ (range, 1┬░ŌĆō9┬░) (Table 3, Fig. 3).
Based on current evidence, spinal tuberculosis is considered as a medical condition, and surgery is required only in the presence of neurological deficits caused by spinal cord compression, disabling back pain, and spinal deformity in spite of ongoing antituberculosis therapy [25611]. Surgical approach in spinal tuberculosis has evolved from anterior to posterior. The anterior approach, popularized by Hodgson [7] in 1960, was advocated traditionally in view of the predilection of the pathology of tuberculosis for the vertebral bodies and disc spaces, and the anterior approach concedes direct access to the infected focus and is convenient for debriding infection and reconstructing the defect [812]. Attainment of bony stability through anterior instrumentation may be insubstantial due to the presence of the concomitant osteoporosis associated with infection of tuberculosis that renders the vertebrae structurally weak and thereby prevents adequate fixation [1314]. A combined anterior plus posterior approach helps to overcome stability-related drawbacks of the anterior approach alone [13141516]. However, it involves two surgeries (can be a single event or performed as a staged procedure), and when performed as a single event, it is associated with increased operative time and more blood loss alongwith exposure of vital structures such as the pleura in already immunocompromised tuberculosis patients, making them susceptible to further infection and thus contributing to further additional morbidity [6]. Campbell et al. [17] have reported higher rates of complications with isolated anterior fixation and combined anterior and posterior spinal fusion in comparison to isolated posterior fusion.
Recently, the transpedicular approach has gained popularity because it is less invasive, allows circumferential cord decompression, can be extended proximally and distally to the involved segment, and providesa stronger three-column fixation through uninvolved posterior elements via pedicle screws [181920]. Functional recovery (evaluated in terms of VAS score) observed in our study was comparable to the results of Sahoo et al. [21] with a mean value of 1.9 at the end of 1 year follow-up. Majority of the patients were pain free at the final follow-up. Significant improvement in neurological grading was evident with an improvement of two grades in more than 50% of cases. Evaluation of radiological healing in cases of spinal tuberculosis has been described by Jain et al. [22] as the remineralization and reappearance of bony trabeculae, sharpening of articular and cortical margins, sclerosis of vertebral body and end plates, and fusion of vertebral bodies on plain X-rays and on MR as resolution of enhanced vertebral body and paravertebral collection and fatty replacement of marrow seen as enhanced intensity on sequential T1 and T2 images. These findings were evident in our study on radiological scans performed at regular intervals. In the present study, loss of correction at the final follow-up was 4.1┬░, which was not statistically significant (p>0.05). This was consistent with the findings of Zhang et al. [23].
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
References
1. World Health Organization. Global tuberculosis control: WHO report 2015. Geneva: World Health Organization; 2015.
2. Trecarichi EM, Di Meco E, Mazzotta V, Fantoni M. Tuberculous spondylodiscitis: epidemiology, clinical features, treatment, and outcome. Eur Rev Med Pharmacol Sci 2012;16(Suppl 2): 58ŌĆō72.
3. Turgut M. Spinal tuberculosis (Pott's disease): its clinical presentation, surgical management, and outcome: a survey study on 694 patients. Neurosurg Rev 2001;24:8ŌĆō13. PMID: 11339471.


4. Nussbaum ES, Rockswold GL, Bergman TA, Erickson DL, Seljeskog EL. Spinal tuberculosis: a diagnostic and management challenge. J Neurosurg 1995;83:243ŌĆō247. PMID: 7616269.


5. Lee TC, Lu K, Yang LC, Huang HY, Liang CL. Transpedicular instrumentation as an adjunct in the treatment of thoracolumbar and lumbar spine tuberculosis with early stage bone destruction. J Neurosurg 1999;91(2 Suppl): 163ŌĆō169.

6. Zaveri G. The role of posterior surgery in spinal tuberculosis. ArgoSpine News J 2011;23:112ŌĆō119.

7. Hodgson AR, Stock FE, Fang HS, Ong GB. Anterior spinal fusion: the operative approach and pathological findings in 412 patients with Pott's disease of the spine. Br J Surg 1960;48:172ŌĆō178. PMID: 13714863.


8. Jain AK, Dhammi IK, Prashad B, Sinha S, Mishra P. Simultaneous anterior decompression and posterior instrumentation of the tuberculous spine using an anterolateral extrapleural approach. J Bone Joint Surg Br 2008;90:1477ŌĆō1481. PMID: 18978269.


10. Frankel HL, Hancock DO, Hyslop G, et al. The value of postural reduction in the initial management of closed injuries of the spine with paraplegia and tetraplegia: I. Paraplegia 1969;7:179ŌĆō192. PMID: 5360915.


11. Khoo LT, Mikawa K, Fessler RG. A surgical revisitation of Pott distemper of the spine. Spine J 2003;3:130ŌĆō145. PMID: 14589227.


12. Benli IT, Kaya A, Acaroglu E. Anterior instrumentation in tuberculous spondylitis: is it effective and safe? Clin Orthop Relat Res 2007;460:108ŌĆō116. PMID: 17452918.


13. Hee HT, Majd ME, Holt RT, Pienkowski D. Better treatment of vertebral osteomyelitis using posterior stabilization and titanium mesh cages. J Spinal Disord Tech 2002;15:149ŌĆō156. PMID: 11927825.


14. Krodel A, Kruger A, Lohscheidt K, Pfahler M, Refior HJ. Anterior debridement, fusion, and extrafocal stabilization in the treatment of osteomyelitis of the spine. J Spinal Disord 1999;12:17ŌĆō26. PMID: 10078945.

15. Fukuta S, Miyamoto K, Masuda T, et al. Two-stage (posterior and anterior) surgical treatment using posterior spinal instrumentation for pyogenic and tuberculotic spondylitis. Spine (Phila Pa 1976) 2003;28:E302ŌĆōE308. PMID: 12897509.


16. Moon MS, Woo YK, Lee KS, Ha KY, Kim SS, Sun DH. Posterior instrumentation and anterior interbody fusion for tuberculous kyphosis of dorsal and lumbar spines. Spine (Phila Pa 1976) 1995;20:1910ŌĆō1916. PMID: 8560340.


17. Campbell PG, Malone J, Yadla S, et al. Early complications related to approach in thoracic and lumbar spine surgery: a single center prospective study. World Neurosurg 2010;73:395ŌĆō401. PMID: 20849799.


18. Moon MS. Combined posterior instrumentation and anterior interbody fusion for active tuberculous kyphosis of the thoraco-lumbar spine. Curr Orthop 1991;5:177.

19. Sundararaj GD, Behera S, Ravi V, Venkatesh K, Cherian VM, Lee V. Role of posterior stabilisation in the management of tuberculosis of the dorsal and lumbar spine. J Bone Joint Surg Br 2003;85:100ŌĆō106. PMID: 12585586.


20. Chacko AG, Moorthy RK, Chandy MJ. The transpedicular approach in the management of thoracic spine tuberculosis: a short-term follow up study. Spine (Phila Pa 1976) 2004;29:E363ŌĆōE367. PMID: 15534398.


21. Sahoo MM, Mahapatra SK, Sethi GC, Dash SK. Posterior-only approach surgery for fixation and decompression of thoracolumbar spinal tuberculosis: a retrospective study. J Spinal Disord Tech 2012;25:E217ŌĆōE223. PMID: 22854920.


22. Jain AK, Srivastava A, Saini NS, Dhammi IK, Sreenivasan R, Kumar S. Efficacy of extended DOTS category I chemotherapy in spinal tuberculosis based on MRI-based healed status. Indian J Orthop 2012;46:633ŌĆō639. PMID: 23325964.



23. Zhang H, Sheng B, Tang M, et al. One-stage surgical treatment for upper thoracic spinal tuberculosis by internal fixation, debridement, and combined interbody and posterior fusion via posterior-only approach. Eur Spine J 2013;22:616ŌĆō623. PMID: 22903198.


Fig.┬Ā2
(A) Preoperative T2 weighted magnetic resonance sagittal image showing D12ŌĆōL1 spondylodiscitis with epidural soft tissue compressing cord. (B) Follow-up magnetic resonance T2 weighted sagittal image at 1 year showing radiological healing (disappearance of soft tissue, fatty marrow conversion).
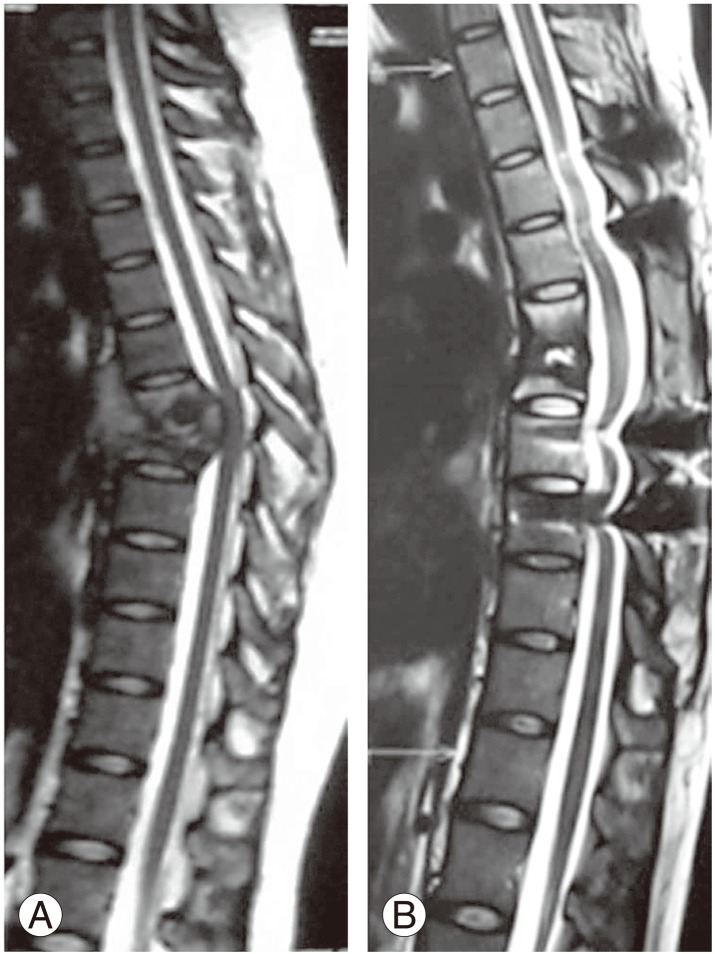
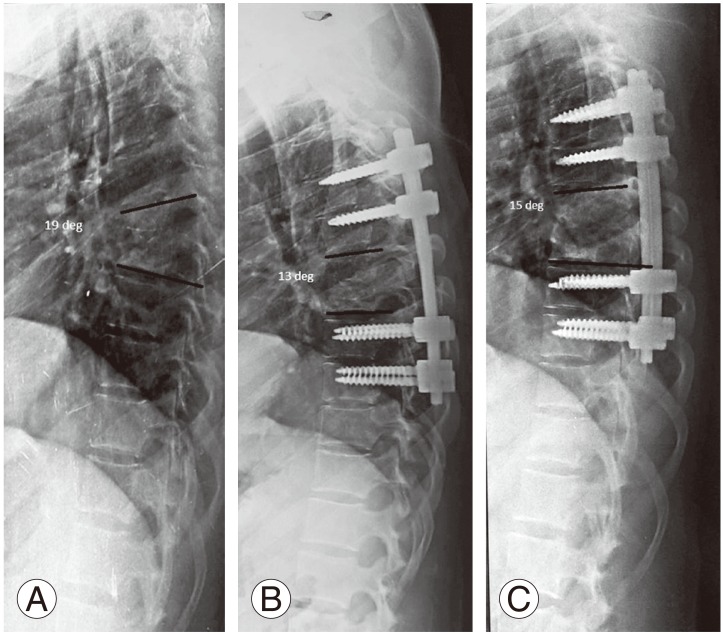
Fig.┬Ā3
(A) Preoperative plain radiograph showing destruction of D12 and L1 with segmental kyphosis of 19┬░. (B) Postoperative radiograph pedicle screws above and below with segmental kyphosis of 13┬░. (C) 1-year follow-up radiograph showing pedicle screws with segmental kyphosis of 15┬░.
- TOOLS
-
METRICS

- Related articles in ASJ
-
Extended Posterior Decompression and Instrumented Fusion for Spinal Tuberculosis2019 December;13(6)