|
 |
- Search
| Asian Spine J > Volume 11(2); 2017 > Article |
|
Abstract
Purpose
Overview of Literature
Methods
Results
Conclusions
Notes
Conflict of Interest: No potential conflict of interest relevant to this article was reported.
References
Fig.┬Ā1
The entry point (X) for the C1 lateral mass screw according to Currier's method. Using a 4-mm burr, the lower portion of the posterior arch (shaded area) is burred until the lateral mass is reached.
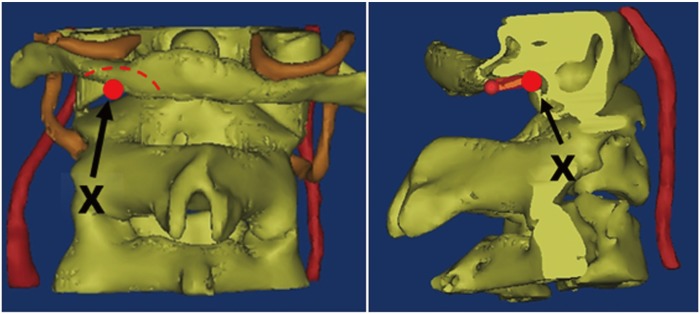
Fig.┬Ā2
Landmarks and measurements on the C1 axial plane, which were resliced according to the neutral sagittal axis of the C1 lateral mass. X represents the entry point of the C1 lateral mass screw. The shortest and longest lengths (SLa and LLa) were represented with small and large dotted lines. The grey and black shaded area represents their corresponding trajectories (SAa and LAa). SLa, shortest length in axial plane; LLa, longest length in axial plane; SAa, angle by shortest length trajectory in axial plane; LAa, angle by longest length trajectory in axial plane.
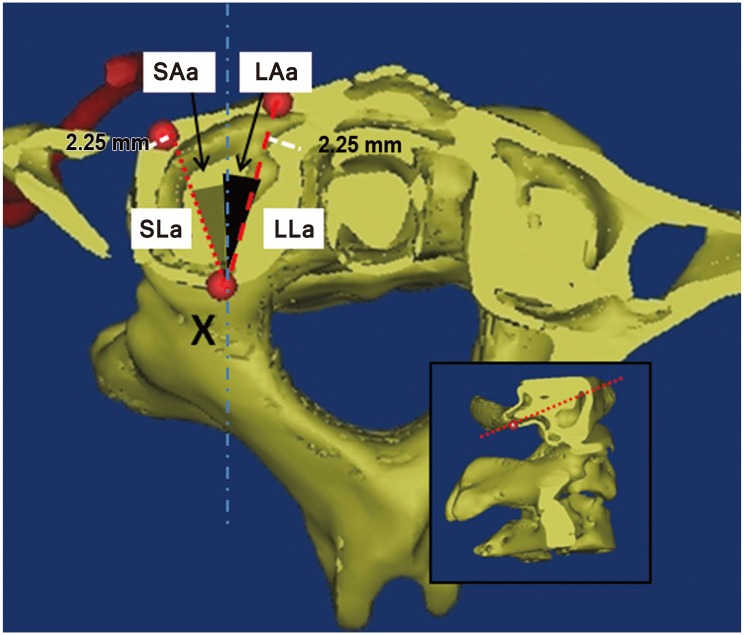
Fig.┬Ā3
Landmarks and measurements on the C1 sagittal plane, which was resliced according to the vertical axis of the C1 lateral mass at X point. The shortest and longest lengths (SLs and LLs) were represented with small and large dotted lines. The grey and black shaded area represents their corresponding trajectories (SAa and LAa). BL, the measurement for base length; SLs, shortest length in sagittal plane; LLs, longest length in sagittal plane; SAs, angle by shortest length trajectory in sagittal plane; LAs, angle by longest length trajectory in sagittal plane.
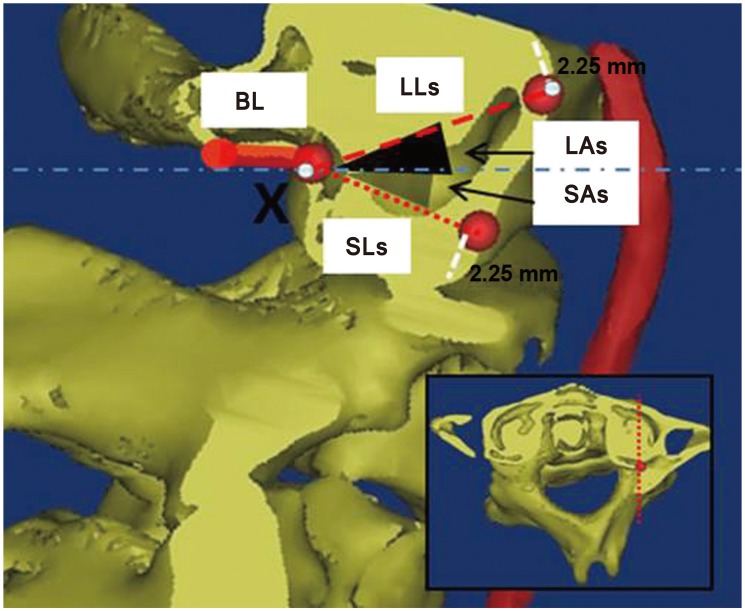
Fig.┬Ā5
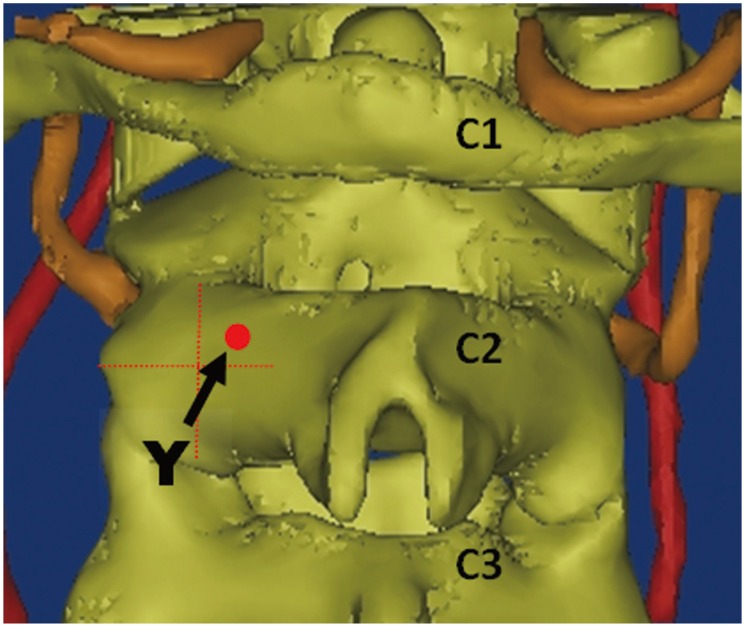
Landmarks and measurements on the C2 axial plane, which was resliced according to the pedicle axis of C2. Y represents the entry point of the C2 pedicle screw. The shortest and longest lengths (SLa and LLa) were represented with small and large dotted lines. The grey and black shaded area represents their corresponding trajectories (SAa and LAa). PAa, to the pedicle axis in the axial plane; SLa, shortest length in axial plane; LLa, longest length in axial plane; SAa, angle by shortest length trajectory in axial plane; LAa, angle by longest length trajectory in axial plane.
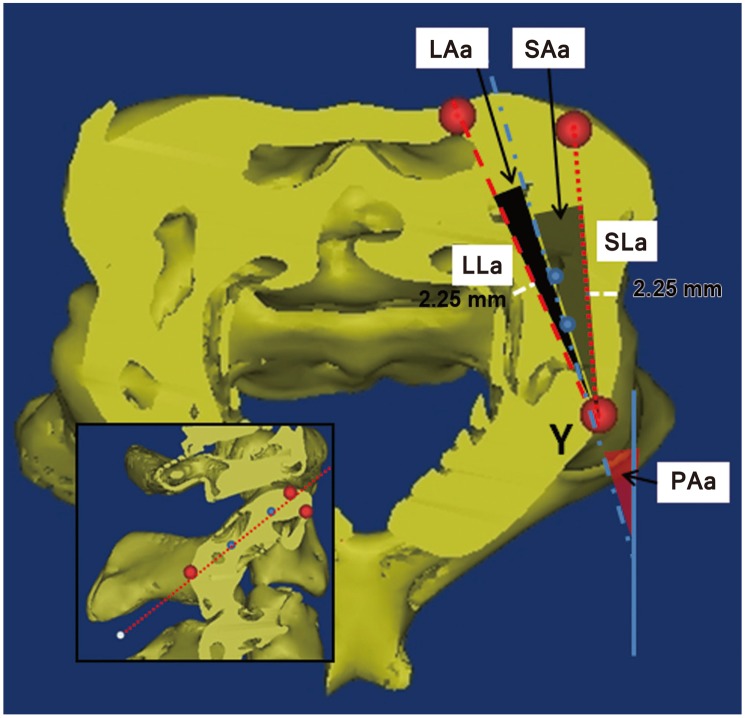
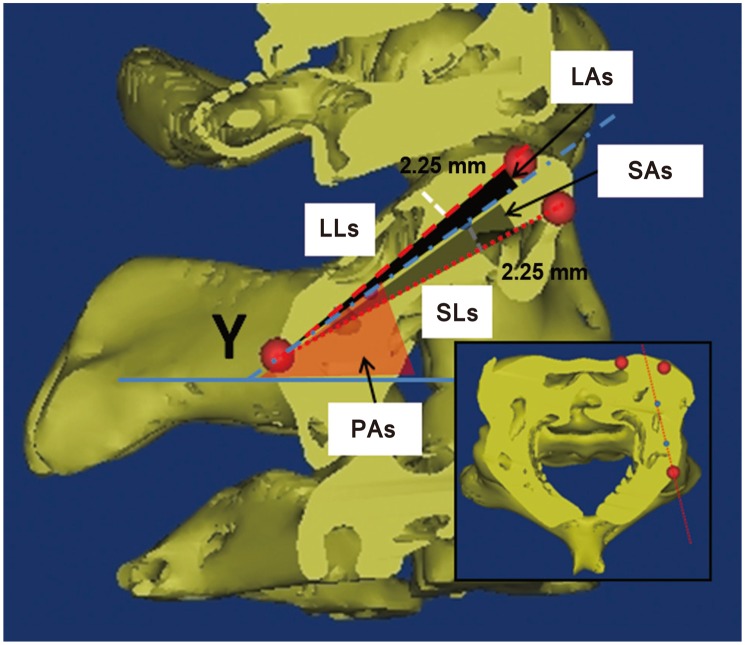
Fig.┬Ā6
Landmarks and measurements on the C2 sagittal plane, which was resliced according to the pedicle axis of C2. The shortest and longest lengths (SLs and LLs) were represented with small and large dotted lines. The grey and black shaded area represents their corresponding trajectories (SAs and LAs). PAs, to the pedicle axis angle in the sagittal plane; SLs, shortest length in sagittal plane; LLs, longest length in sagittal plane; SAs, angle by shortest length trajectory in sagittal plane; LAs, angle by longest length trajectory in sagittal plane.
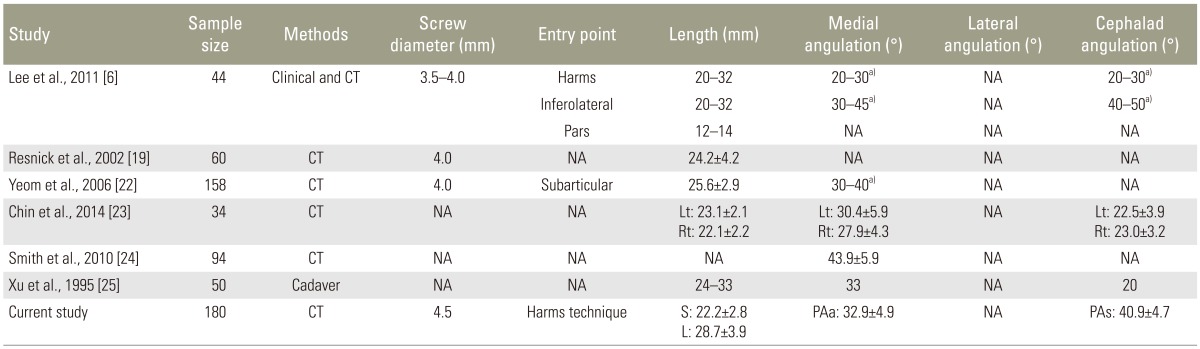
Table┬Ā1
C1 parameters in length and angulations, and their comparisons in between genders, sides and races

Values are presented as mean┬▒standard deviation.
SLa, shortest length in axial plane; LLa, longest length in axial plane; SLs, shortest length in sagittal plane; LLs, longest length in sagittal plane; BL, base length; SAa, angle by shortest length trajectory in axial plane; LAa, angle by longest length trajectory in axial plane; TAa, the safe zone in the axial plane; SAs, angle by shortest length trajectory in sagittal plane; LAs, angle by longest length trajectory in sagittal plane; TAs, the safe zone in the sagittal plane.
Table┬Ā3
C2 parameters in length and angulations, and their comparisons in between genders, sides and races
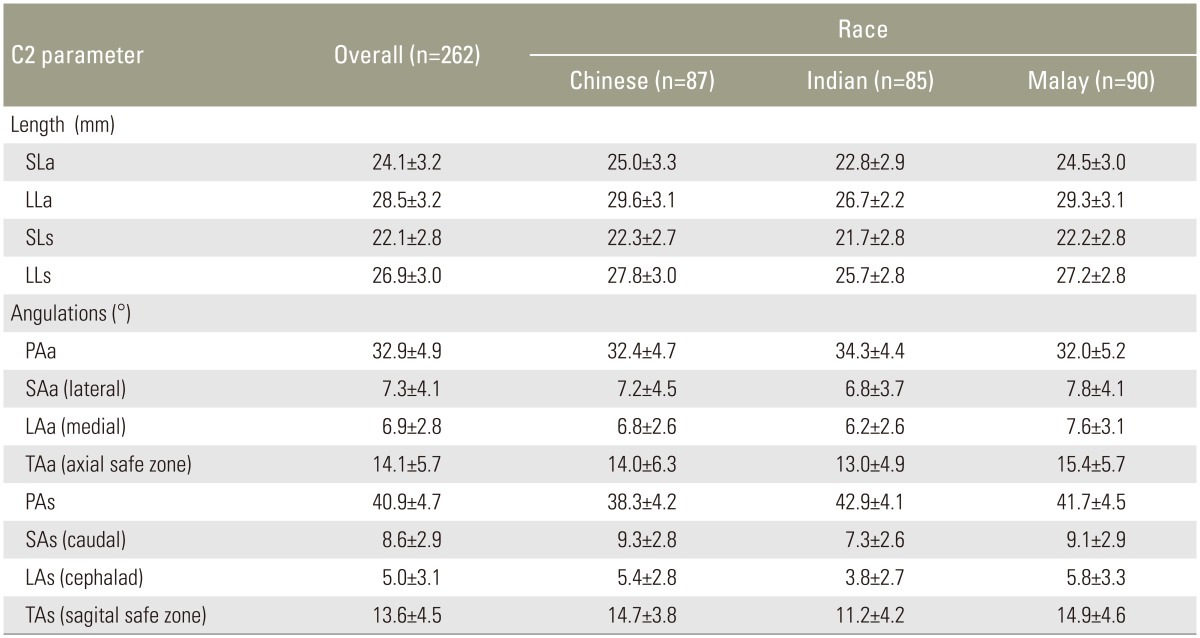
Values are presented as mean┬▒standard deviation.
SLa, shortest length in axial plane; LLa, longest length in axial plane; SLs, shortest length in sagittal plane; LLs, longest length in sagittal plane; PAa, pedicle axis in the axial plane; SAa, angle by shortest length trajectory in axial plane; LAa, angle by longest length trajectory in axial plane; TAa, the safe zone in the axial plane; PAs, pedicle axis in the sagittal plane; SAs, angle by shortest length trajectory in sagittal plane; LAs, angle by longest length trajectory in sagittal plane; TAs, the safe zone in the sagittal plane.
- TOOLS