Incidence and Characteristics of Clinical L5–S1 Adjacent Segment Degeneration after L5 Floating Lumbar Fusion: A Multicenter Study
Article information
Abstract
Study Design
Retrospective study.
Purpose
This study aimed to evaluate the incidence, characteristics, and risk factors for clinical L5–S1 adjacent segment degeneration (ASD) after L5 floating lumbar fusion.
Overview of Literature
ASD is known to occur after lumbar spine fusion at a certain frequency. Several studies on radiological L5–S1 ASD have been reported. However, there are only a few studies on L5–S1 ASD with clinical symptoms, including back pain and/or radiculopathy.
Methods
In total, 306 patients who received L5 floating lumbar fusion were included in this study. Clinical L5–S1 ASD was defined as newly developed radiculopathy in relation to the L5–S1 segment. Patients’ medical records and imaging data were retrospectively analyzed. The risk factors for clinical ASD were assessed by an inverse probability of treatment weighting-adjusted logistic regression analysis.
Results
Clinical L5–S1 ASD occurred in 17 patients (5.6%). The mean onset time of L5–S1 ASD was 12.9±7.5 months after the primary surgery. Among these patients, 10 (58.8%) presented with clinical L5–S1 ASD within 12 months. Reoperation was performed in three patients (1.0%). The severity of L5–S1 disk degeneration did not affect the occurrence of L5–S1 ASD. Logistic regression analysis showed that the number of fusion levels was a significant risk factor for clinical L5–S1 ASD.
Conclusions
The incidence and characteristics of clinical L5–S1 ASD after L5 floating lumbar fusion were retrospectively investigated. This study established that the number of fusion levels was a significant candidate factor for clinical L5–S1 ASD. Careful clinical follow-up is deemed necessary after L5 floating lumbar fusion surgery, especially for patients who received multiple-level fusions.
Introduction
Lumbar fusion, which aims to relieve back pain attributed to movement at intervertebral structures and increase intervertebral disk height and foramen space, is considered a stabilizing treatment that significantly improves the surgical outcomes for patients with degenerative lumbar diseases. The use of lumbar fusion surgeries has grown dramatically in the past decades [1,2].
However, adjacent segment degeneration (ASD) occurs after lumbar spine fusion at a certain frequency due to increases in intervertebral stress and adjacent segment motions [3–5]. As per a systematic review [6], the occurrence of radiographic and clinical ASD after lumbar spinal fusion surgery ranges from 5% to 77% and from 0% to 27%, with a pooled prevalence of 26.6% and 8.5%, respectively.
The L5–S1 segment has a distinctive segmental motion and biomechanical properties that differ from other lumbar segments [7,8]. The iliolumbar ligament is described as a ligamentous structure in the lumbosacral region that firmly binds the L5–S1 segment and/or sacroiliac joint. The iliolumbar ligament has been described as the most important ligament for restraining movement at the lumbosacral junction [9,10]. Clinically, the incidence of cranial ASD after spinal fusion extending to the sacrum is significantly higher than after L5 floating fusion [11]. A biomechanical study using finite element models demonstrated that more distal fusion levels, particularly in spinal fusion, including the L5–S1 level, can lead to a greater risk of proximal junctional kyphosis and failure [12]. Therefore, there has been controversy about whether the L5–S1 segment without clinical symptoms should be included in the fusion segment. Although studies on radiological L5–S1 ASD have been reported [13–15], only a few studies have been reported on L5–S1 ASD with clinical symptoms, including low back pain and neuropathic pain (clinical L5–S1 ASD).
Therefore, this retrospective study has aimed to evaluate the incidence, characteristics, and risk factors for clinical L5–S1 ASD after L5 floating lumbar fusion in a multicenter study.
Materials and Methods
1. Subjects
This study was approved by the Ethics Committee of Mie University Hospital (Tsu, Japan; institutional review board reference no., H2020-028). Informed consent was obtained in the form of optout on the website. Lumbar spinal fusions were performed for 497 patients between April 2007 and June 2017 in three institutions. Among these, 306 patients (61.6%) who received L5 floating lumbar fusion were included in this study. Preoperative diagnoses for L5 floating surgery were degenerative spondylolisthesis (n=198), lumbar spinal stenosis (LSS; n=75), LSS with degenerative scoliosis (Cobb angle <20°; n=19), LSS with vertebral fracture (n=6), LSS with disk herniation (n=5), and LSS with spondylolysis (n=3). The inclusion criteria for subjects of this study were those patients who (1) underwent L5 floating fusion (the upper instrumented vertebra [UIV] was L1–L4, and the lower instrumented vertebra was L5) and (2) had a follow-up period of >12 months. The exclusion criteria for subjects of this study included those patients who underwent (1) reoperation, (2) decompression at L5–S1, (3) degenerative scoliosis (Cobb angle >20°), (4) long fusion across the thoracolumbar spine, and (5) operation for malignant disease. The medical records and imaging data of patients who received L5 floating lumbar fusion were retrospectively analyzed.
Clinical L5–S1 ASD was defined as newly developed back pain and/or radiculopathy in relation to the L5–S1 segment, including disk herniation, canal stenosis, and foraminal stenosis, as identified by computed tomography (CT) and/or magnetic resonance imaging (MRI) without significant canal stenosis at the L4–L5 level [8]. A representative case is shown in Fig. 1.
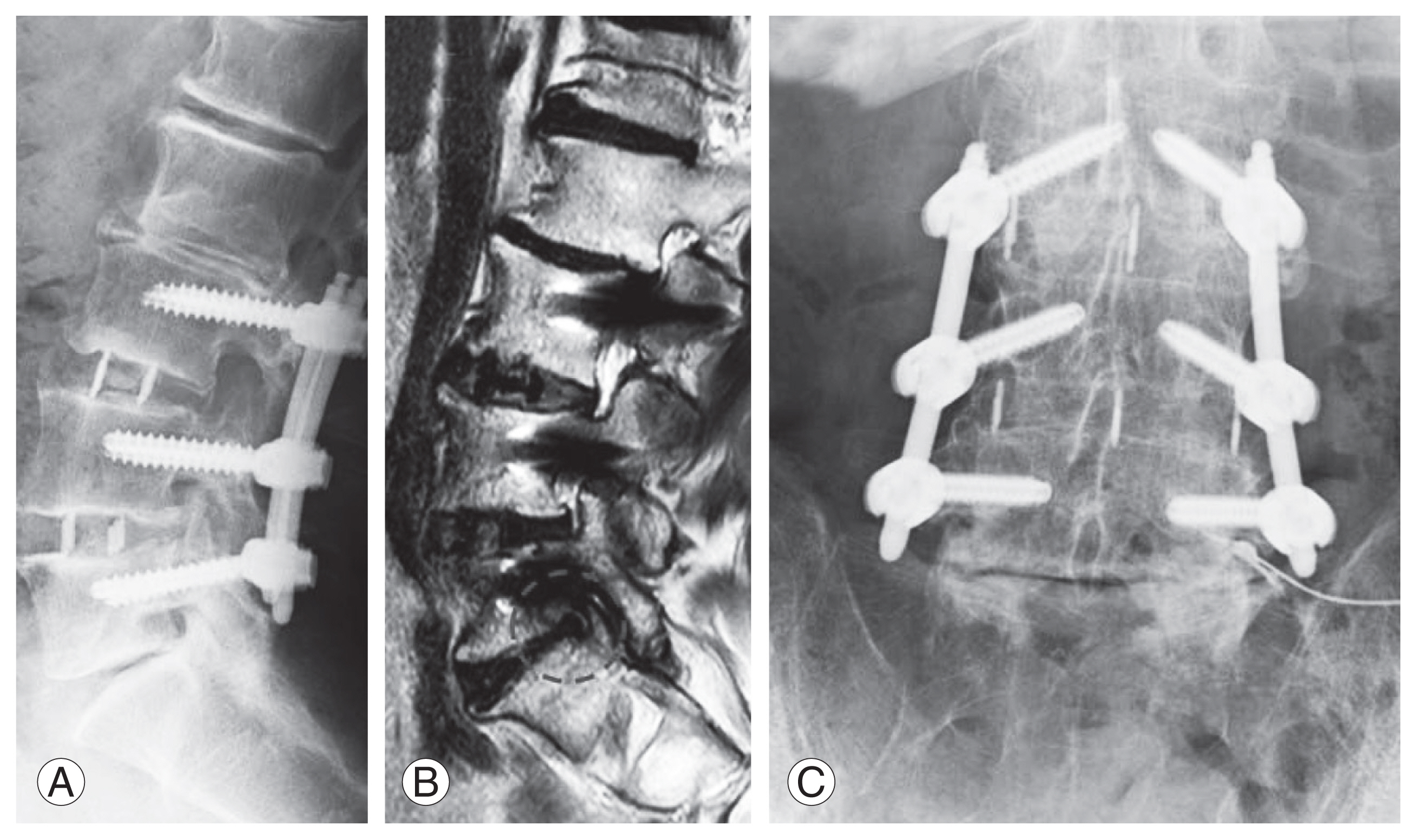
Representative case of clinical L5–S1 adjacent segment degeneration (ASD). A 68-year-old man received lateral lumbar interbody fusion with pedicle screw fixation from L3 to L5 for lumbar spinal stenosis. Adjacent segment degeneration at L5–S1 occurred 5 months after surgery. (A) Postoperative lumbar lateral radiograph. (B) Magnetic resonance imaging (MRI) examination was performed when neurological symptoms occurred 5 months after surgery. Right foraminal stenosis at L5–S1 was identified by MRI examination (dotted circle). (C) Right L5 spinal nerve block was performed under X-ray fluoroscopy.
The following items were evaluated: age at primary operation, gender, body mass index (BMI), medical complications (hypertension, diabetes mellitus, osteoporosis, and use of immunosuppressive agent), preoperative Japanese Orthopedic Association (JOA) score [16,17], preoperative L5–S1 disk degeneration, number of fusion levels, operative procedure, onset time of clinical symptoms, and medical treatment for clinical symptoms. The JOA score consisted of scores for low back pain, leg pain, walking distance, straight leg raising, sensory deficit, motor deficit, activities of daily living, and urological symptoms [16,17].
2. Control groups
To identify the risk factors for clinical ASD, a control group was isolated from patients without ASD who were matched in a 1:2 manner to the ASD patients according to age, gender, and follow-up duration; however, the groups were not matched by body height, body weight, BMI, operative procedure, and number of fusion levels, as reported previously [18]. There were no significant differences in terms of age, gender, body height, body weight, BMI, operation procedure, number of fusion levels, and follow-up period between the control and nonASD patients.
3. Classification of disk degeneration
The degree of disk degeneration was evaluated by sagittal T2-weighted lumbar MRI and graded according to Pfirrmann’s classification from grades I to V [19]. Grades II and III were defined as early stages of intervertebral disk degeneration, and grades IV and V were defined as advanced stages, as reported previously [20,21].
4. Diagnosis of vacuum phenomenon
To evaluate disk ruptures associated with disk degeneration, intradiscal vacuum phenomena (VPs) were evaluated by the presence of areas of gaseous radiolucency using multidetector CT imaging, as has been previously reported [20].
5. Statistical analysis
The Student t-test was used to determine the differences in the number of fusion levels, body height, body weight, and BMI between the ASD and control groups. The differences in medical complications, preoperative L5–S1 disk degeneration, and preoperative L5–S1 intradiscal VP between the ASD and control groups were analyzed using the χ2 test. The inverse probability of treatment weighting (IPTW) using the propensity score was applied to balance the ASD and control groups for their patient and treatment characteristics [22,23]. This method uses weights based on the propensity score to create a synthetic sample, in which the distribution of measured baseline and treatment covariates is independent of the group assignment. In this way, the patient groups are made similar to each other, and outcome measures can be compared between similar patients. The propensity score was estimated without regard to outcome variables using multiple logistic regression analysis. To evaluate the risk factors for clinical L5–S1 ASD, bivariate comparisons of patient characteristics in the patient groups after IPTW adjustment were performed using general linear modeling. “Operative procedure” was excluded from the candidate factors because there was a statistically significant relationship between “operative procedure” and “number of fusion levels.” All statistical analyses were performed using IBM SPSS Statistics ver. 24.0 (IBM Corp., Armonk, NY, USA). Significance was accepted at p<0.05.
Results
L5–S1 ASD with neurological manifestation in the lower extremities occurred in 17 patients (5.6%) after L5 floating lumbar fusion (Table 1).
The mean age at the time of surgery was 67.1±9.8 years. The preoperative mean JOA score was 11.2±4.8. The mean onset time of L5–S1 ASD was 12.9±7.5 months after the primary surgery. In ten patients (58.8%), clinical L5–S1 ASD occurred within 1 year after the primary surgery. Conservative treatments were performed in 14 patients (82.4%), and reoperation was performed in three patients (17.6%).
MRI analysis showed the early stage of degeneration (Pfirrmann grades II and III) in the preoperative L5–S1 disk in 11 patients (64.7%) and the advanced stage (Pfirrmann grades IV and V) in six patients (35.3%) (Fig. 2A). CT analysis showed the presence of intradiscal VP in the preoperative L5–S1 disk in six patients (35.3%) (Fig. 2B).
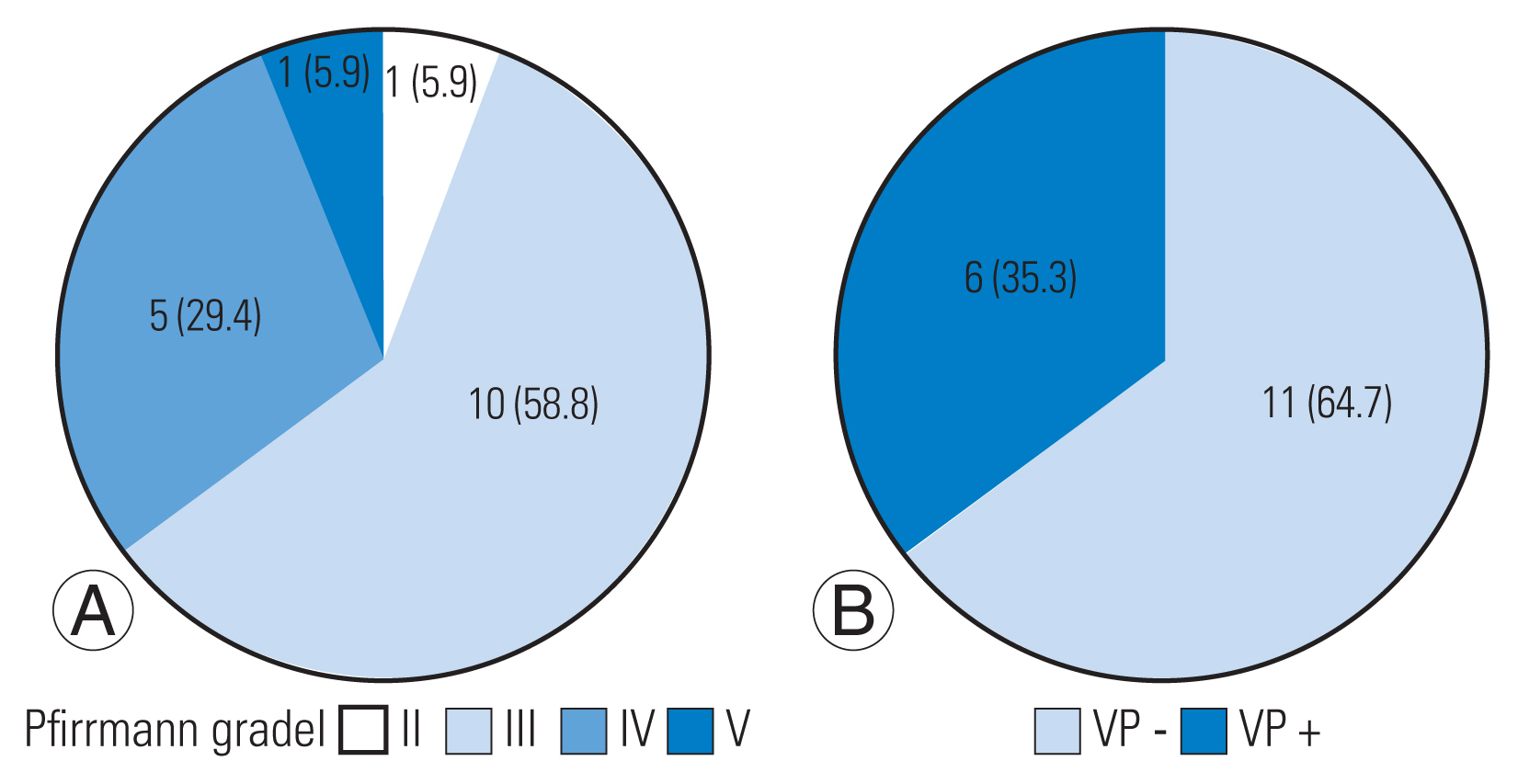
The extent of preoperative disc degeneration of clinical L5–S1 adjacent segment degeneration patients. (A) Magnetic resonance imaging analysis showed early-stage degeneration (Pfirrmann grades II and III) in the preoperative L5–S1 disc in 11 patients (64.7%) and advanced stage degeneration (Pfirrmann grades IV and V) in six patients (35.3%). (B) Computed tomography analysis showed that intradiscal vacuum phenomenon (VP) was present in the preoperative L5–S1 disc in six patients (35.3%). Values are presented as number (%).
Thirty-four patients (16 males and 18 females) were enrolled as the control group (Table 2). The mean age of the control group was 69.7±8.5 years, and the mean number of fusion levels of the control group was 1.6±0.7. Seven patients in the control group received lateral lumbar interbody fusion (LLIF), whereas 27 patients received posterior lumbar interbody fusion (PLIF). There were no significant differences in terms of age, gender, number of fusion levels, BMI, medical complications, preoperative L5–S1disc degeneration, and preoperative L5–S1 intradiscal VP between the control and ASD groups (Table 2).
IPTW-adjusted logistic regression analysis showed that the number of fusion levels was a significant factor associated with clinical L5–S1 ASD groups (Table 3).
Discussion
The incidence and characteristics of clinical L5–S1 ASD after L5 floating lumbar fusion were retrospectively investigated. The incidence was 5.6%, and the reoperation rate was 1.0%.
The six clinical studies that evaluated clinical L5–S1 ASD are summarized in Table 4. According to these studies, the incidence of clinical ASD was 5.2%–8.7% [8,24,25], and the reoperation rate was 1.6%–4.8% [4,8,11,24–26]. These incidences were comparable to those in this study.
Ushio et al. [26] evaluated patients who underwent floating fusion surgery at vertebrae L3–L5, whereas Choi et al. [25] and Ghiselli et al. [27] investigated patients who underwent lumbar fusion only at the L4–L5 segment. In the other studies, the UIV was not determined; this was similar to the criteria of this study. The number of subjects in this study (306 patients who underwent L5 floating lumbar fusion) was significantly higher than those in previous studies; therefore, the large sample size was a strength of this study. In this study, the IPTW-adjusted logistic regression analysis showed that the number of fusion levels was the significant factor associated with clinical L5–S1 ASD. Therefore, the number of fusion levels may be the most important factor associated with clinical L5–S1 ASD development. Many LLIF surgeries were performed for multilevel fusion in this series, and the number of fusion levels in patients who received LLIF was significantly higher than in patients who received PLIF/posterolateral fusion (data not shown).
The risk factors for L5–S1 clinical ASD were evaluated in three studies [8,24,25]. Lee et al. [8] concluded that preoperative spinal stenosis of the L5–S1 segment was a risk factor for clinical ASD; however, the incidence of L5–S1 ASD (8.7%) and reoperation rate (4.3%) in their study was higher than those in this and other studies. Although spinal stenosis was not evaluated in this study, patients with spinal stenosis at the L5–S1 segment before surgery might have undergone decompression and/or fusion surgeries in this series dependent on the surgeon’s decision.
Choi et al. [25] evaluated L5–S1 ASD after L4–L5 interbody fusion and determined whether preexisting L5–S1 degeneration influenced radiological and clinical outcomes. They reported that clinical ASD at L5–S1 occurred in three patients (5.2%) and that one patient (1.7%) required surgery. Clinical ASD developed in one patient (4.5%) in the group with preexisting degeneration and two patients (5.7%) in the group without preexisting degeneration. They concluded that preexisting L5–S1 degeneration did not affect the occurrence of clinical and radiological ASD after isolated L4–5 fusion. Similarly, this study showed that L5–S1 clinical ASD occurred in patients with early-stage disk degeneration at L5–S1 before surgery. Choi et al. [25] and this study suggested that preoperative disk degeneration may not be associated with the development of clinical ASD. This study also evaluated intradiscal VPs using CT analysis for evaluation of disk rupture associated with disk degeneration and found no significant association between preoperative intradiscal VPs and the occurrence of clinical ASD.
Orita et al. [24] reported that multivariate logistic regression analysis of possible risk factors for L5–S1 ASD revealed that gender (male), L5–S1 wedging angle, foraminal ratio, and multilevel fusion were statistically significant. In their study, the candidate risk factors were evaluated by radiographic parameters, including the wedging angle of L5–S1 in the frontal view, lumbosacral height in the sagittal view in standing lumbar X-ray images, and bilateral foraminal ratio in sagittal T1 WI in MRI. The differences in evaluation criteria could lead to different results between this study and Orita et al. [24].
Only one study reported that the average onset time of L5–S1 clinical ASD was 13.3 months after the primary surgery [24]. In this study, the mean onset time of L5–S1 clinical ASD was 12.9±7.5 months after the surgery. Importantly, 10 patients (55.6%) in this cohort suffered from symptoms of L5–S1 clinical ASD within 1 year after the surgery, which is a relatively shorter time.
This study has some limitations. First, because this study was retrospective, the criteria for performing L5–S1 fusion at the primary surgery were not unified. Second, the degree of preoperative foraminal stenosis, central stenosis, and facet joint degeneration at the L5–S1 level was not evaluated preoperatively. Third, preoperative and postoperative spinal alignments that might influence L5–S1 ASD were not evaluated. Finally, the degenerative changes of the L5–S1 disk at ASD onset were not evaluated. Therefore, the temporal changes of L5–S1 disk degeneration after L5 floating fusion remain unknown.
Conclusions
This was a retrospective multicenter study for the incidence of clinical L5–S1 ASD after L5 floating lumbar fusion with the highest number of subjects compared to previous studies. The incidence of clinical L5–S1 ASD was 5.6%, and the reoperation ratio was 1.0%. Furthermore, the onset time of L5–S1 ASD of >50% of subjects was within 1 year after the primary surgery. Interestingly, the severity of L5–S1 disk degeneration did not contribute to the onset of clinical L5–S1 ASD. This study has identified that the number of fusion levels was a significant risk factor for clinical L5–S1 ASD. Careful clinical follow-up after L5 floating lumbar fusion, especially for patients who received multiple-level fusions, is necessary because L5–S1 ASD could develop relatively early after the surgery, even in cases without preoperative L5–S1 disk degeneration.
Notes
Conflict of Interest
No potential conflict of interest relevant to this article was reported.
Author Contributions
NT performed data acquisition and statistical analysis and drafted the manuscript. KA helped with data acquisition and statistical analyses, drafted the manuscript, conceived this study, and made substantial contributions to the study design. JY, TI, TF, TK, and KT performed data acquisition, and revised the manuscript. AS contributed to the study design and coordination and revised the manuscript. All authors contributed to the data analysis, drafting or revising the article, agreed on the journal, to which the article will be submitted, gave final approval of the version to be published, and agreed to be accountable for all aspects of the work.



