 |
 |
- Search
| Asian Spine J > Volume 15(6); 2021 > Article |
|
Abstract
Purpose
To evaluate lumbar disc degeneration (LDD) on magnetic resonance imaging (MRI) in symptomatic subjects to accumulate baseline data on the pattern of degeneration.
Overview of Literature
LDD plays an important role in the diagnosis and treatment of low-back pain in patients. Few studies have focused on the pattern of LDD to understand how the lumbar spine ages.
Methods
This study included 1,095 patients (mean age, 44.29 years; range, 16ŌĆō85 years) who underwent upright lumbar MRI. LDD was graded into five categories (IŌĆōV). Positive LDD was defined as grade III or greater. The prevalence and pattern of LDD were analyzed, and the correlations between age and total grade of LDD were evaluated.
Results
The average number of LDD levels and the total grade of LDD increased with age. LDD moved cephalad with age. The rate of LDD increased rapidly during the decade before the prevalence of LDD and became >50%. In the single-level LDD group, the levels L5ŌĆōS1 were the most common levels (60.3%). In the two-level group, L4ŌĆōL5 and L5ŌĆōS1 were the most common levels (53.5%). In the three-level group, L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1 were the most common levels (55.7%). In the multilevel LDD group, contiguous multilevel disc degeneration (CMDD) was more common than the skipped level disc degeneration (SLDD). The levels L4ŌĆōL5 were the most common levels in the CMDD group, and L5ŌĆōS1 were the most common levels among SLDD.
Intervertebral lumbar disc degeneration (LDD) is a common finding on magnetic resonance imaging (MRI). The prevalence of LDD was reported to range from 26%ŌĆō91% depending on the age of the patient population [1ŌĆō5].
The reported association between low-back pain and LDD ranged from mild to strong [1,3,6,7]. Lumbar spinal fusion is the mainstay spine procedure for treatment of patients with lumbar diseases. However, adjacent segment disease (ASD) is a condition that often develops after fusion procedure. The prevalence of ASD ranged from lower than 10% to nearly 100% [8ŌĆō10]. Many different motion-sparing procedures have been developed to reduce the incidence of ASD [11,12]. A recent meta-analysis conducted by Pan et al. [13] investigated the efficacy of these procedures to reduce the prevalence of ASD compared with lumbar fusion. However, the rate of ASD was still as high as 18.6%. The cause of ASD was reported to be a combination of processes related to both biomechanical stress and the natural progression of the disease [9,14,15]. The relative scarcity of data, and the observed variations in the reported evidence make it difficult to develop a conclusive understanding of LDD.
In addition to the understanding the structural changes of LDD, we must also learn and understand the pattern of LDD relative to the number of levels of LDD, and the combinations of lumbar levels involved. This information will help us predict the pattern of LDD, and may improve our ability to customize treatment to the needs of individual patients.
MRI is the gold standard investigation for evaluating LDD. MRI demonstrated an ability to precisely evaluate LDD, and to yield information needed to accurately and reliably classify the severity of LDD [16]. The aim of this study was to evaluate LDD on MRI in a large cohort of symptomatic subjects with low-back pain to accumulate baseline data on the pattern of LDD to better understand how the lumbar spine ages.
This cross-sectional study included patients who were referred for upright MRI owing to complaints of low-back pain with or without leg pain. The Institutional Review Board of the University of California Los Angeles approved this study (approval no., 10-000968), and informed consent was obtained from all participants.
A total of 1,169 patients (507 females, 662 males) were included with a mean age of 44.29 years (range, 16ŌĆō85 years). Patients with a previous history of spinal surgery or vertebral fracture, or who had incomplete or poor imaging outcomes were excluded.
MRI of the lumbar spine was performed using a 0.6 Tesla MRI scanner (UPRIGHT Multi-Position; Fonar Corp., Melville, NY, USA). Two vertically oriented opposing magnetic doughnuts placed 45.72 cm apart were used that facilitated scanning of the patients in an upright, axially loaded position. A planar quadrature channel radiofrequency coil was used to acquire images. We examined the longitudinal relaxation (T1)-weighted sagittal spin echo images (repetition time, 671 ms; echo time, 17 ms; slice thickness, 4.0 mm; field-of-view, 30 cm; matrix, 256├Ś224; number of excitations [NEX], 2) and transverse relaxation (T2)-weighted fast spin echo images (repetition time, 3,000 ms; echo time, 140 ms; thickness, 4.0 mm; field-of-view, 30 cm; matrix, 256├Ś224; NEX, 2) for all patients.
We measured all functional lumbar spinal levels, including L1ŌĆōL2, L2ŌĆōL3, L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1. Four spine surgeons graded the degree of disc degeneration into five grades using T2-weighted neutral sagittal images according to the grading system proposed by Pfirrmann et al. [16] (Table 1).
Intraobserver and interobserver agreement for grading of the included intervertebral discs was determined using MRI from 100 randomly selected subjects. The reliability of MRI grading was estimated using agreement percentages and kappa statistics for each observer (intraobserver reliability), and among the four spine surgeons (interobserver reliability).
A total of 5,845 lumbar intervertebral discs were classified into five grades according to the criteria set forth in the Pfirrmann grading system by the same four spine surgeons [16]. The prevalence of degenerative disc grading at each lumbar level was assessed. The total LDD (total LDD) score was calculated by summarizing the degenerative disc score of all lumbar levels (L1ŌĆōL2, L2ŌĆōL3, L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1) in each patient. The correlation between total LDD and age was evaluated. Age decade was defined as follows: 10s, 11ŌĆō20 years; 20s, 21ŌĆō30 years; 30s, 31ŌĆō40 years; 40s, 41ŌĆō50 years; 50s, 51ŌĆō60 years; 60s, 61ŌĆō70 years; and 70s, Ōēź71 years.
Discs that were classified as Pfirrmann grades I or II were defined as nonlumbar disc degeneration states. Alternatively, discs that were graded as Pfirrmann grade III, IV, or V were defined as significant LDD states. The number of lumbar levels of LDD was also assessed. Accordingly, patients were classified as single-, two-, three-, four-, or five-level LDDs. The prevalence of the number of levels of LDD was also analyzed.
Multilevel lumbar disc degeneration (more than two levels of disc degeneration) was further classified as skipped level lumbar disc degeneration (SLDD) or contiguous multilevel lumbar disc degeneration (CMDD). SLDD was defined as skipped or noncontiguous, multilevel involvement, and CMDD was defined as multilevel involvement that affects immediately adjacent lumbar levels [3]. The prevalence of SLDD and CMDD was assessed based on the number of levels affected, and the specific combinations of levels affected.
All statistical analyses were performed using IBM SPSS software ver. 20.0 (IBM Corp., Armonk, NY, USA). PearsonŌĆÖs correlation coefficient was used to analyze the correlation between the patient age and total disc degeneration score, number of levels of disc degeneration, and degree of disc degeneration. The pattern of disc degeneration was analyzed using chi-square tests. Categorical data are presented as number and percentage. The level of statistical significance was set at p<0.05.
Intraobserver agreement of the four observers was excellent with kappa values ranging from 0.84 to 0.94. Interobserver agreement among the four reviewers was good to excellent with kappa values ranging from 0.77 to 0.90.
Total disc degeneration score showed a moderate positive correlation with increasing age (PearsonŌĆÖs correlation coefficient: 0.649; p<0.001) (Fig. 1). The degree of degeneration at each lumbar level exhibited mild to moderate correlation with aging (PearsonŌĆÖs correlation coefficients: L1ŌĆōL2, 0.42; L2ŌĆōL3, 0.49; L3ŌĆōL4, 0.55; L4ŌĆōL5, 0.48; and L5ŌĆōS1, 0.36; p<0.001). Moderate correlation was observed between aging and the number of affected lumbar levels (PearsonŌĆÖs correlation coefficient: 0.60; p<0.5).
Regarding the percentage of LDD at each lumbar level, the percentages tended to increase with age for all lumbar levels (Fig. 2). Caudad levels degenerated earlier than cephalad levels. Specifically, the data showed that the percentage of LDD was >50% at an in earlier age at the caudad levels than at the cephalad level (i.e., L5ŌĆōS1 during the 30s, L4ŌĆōL5 during the 40s, L3ŌĆōL4 during the 50s, and L1ŌĆōL2 and L2ŌĆōL3 during the 60s).
Interestingly, the rates of disc degeneration increased rapidly during the decade before the prevalence of LDD became greater than 50% for all lumbar levels. L1ŌĆōL2 and L2ŌĆōL3 from the 50s to the 60s had the highest percentage increase in disc degeneration (30.47% and 27.56%, sequentially). The percentage of LDD at L3ŌĆōL4 increased rapidly (26.78%) from the 40s to the 50s. The LDD at L4ŌĆōL5 increased rapidly (20.36%) from the 30s to the 40s. LDD at L5ŌĆōS1 increased markedly (14.85%) from the 20s to the 30s. The greatest increase in LDD at L5ŌĆōS1 was observed from the 60s to the 70s (16.47%).
LDD started as early as the first decade of life, and these individuals had LDD less than 50% after their 20s. The prevalence of single-level LDD increased from the first decade of life to its peak during the 30s. Two-level LDD increased gradually from young age to its peak during the 50s, and then there was a sudden decrease during the 60s. Three-level LDD started from the 20s to its peak during the 50s, and then three-level LDD became greater than two-level LDD during their 60s and 70s. Four-level LDD started during the third decade of life and increased slowly to the sixth decade, and then rapidly increased during the seventh decade. Five-level LDD started during the 30s and increased rapidly from the 50s to the 60s. Greater than 50% of our study population had been diagnosed with five-level LDD at ages >60 years (Fig. 3).
In single-level LDD, the most common level was L5ŌĆōS1. In multilevel LDD, the highest percentage increase moved cephalad from L4ŌĆōL5 to L1ŌĆōL2, in addition to a single-level increase in disc degeneration (Table 2). In two-level LDD, the highest increasing percentage from one-level LDD (49.01%) occurred at L4ŌĆōL5. In three-level LDD, the highest percentage increase from two-level LDD (47.09%) was observed at L3ŌĆōL4. In four-level LDD, the highest increasing percentage from three-level LDD (49.57%) took place at L2ŌĆōL3. In five-level LDD, the highest percentage increase from four-level LDD (50.49%) was identified at L1ŌĆōL2. Among multilevel LDD, CMDD (n=485) was more common than SLDD (n=131) (ratio, 7.3:2.7) (Table 3).
Among the CMDD group, the most common combinations were among the caudad levels, as follows: L4ŌĆōL5 and L5ŌĆōS1 (53.50%) in two-level LDD; L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1 (55.70%) in three-level LDD; and, L2ŌĆōL3, L3ŌĆōL4, L4ŌĆōL5, and L5vS1 (50.48%) in four-level LDD. Interestingly, the most common lumbar disc level in CMDD was L4ŌĆōL5 (96.28%), not L5ŌĆōS1 (54.64%).
In SLDD, the most common combinations were the combination of caudad levels with one normal level preserved disc next to the uppermost degenerative disc, as follows: L3ŌĆōL4 and L5ŌĆōS1 (11.52%) in two-level LDD; L2ŌĆōL3, L4ŌĆōL5, and L5ŌĆōS1 (10.74%) in three-level LDD; and L1ŌĆōL2, L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1 (15.53%) in four-level LDD. The most common LDD in SLDD was L5ŌĆōS1 (89.31%).
This cross-sectional study showed baseline of patterns of LDD in symptomatic patients, and the characteristics of LDDŌĆömainly specific to lumbar levelŌĆöwere reported. These findings may help surgeons to understand the patterns of LDD in symptomatic patients. Correspondingly, this information may enhance individual treatment planning and improve patient outcomes.
Aging is a factor that is commonly reported to be associated with disc degeneration [2,3,17ŌĆō20]. Consistent with these findings, the present study also found that aging was significantly associated with the total LDD score. In addition to total LDD score, we also found aging to be associated with both degree of disc degeneration and number of levels of LDD. The decade of age when the percentage of LDD became greater than 50% (L5ŌĆōS1 during the 30s, L4ŌĆōL5 during the 40s, L3ŌĆōL4 during the 50s, and L1ŌĆōL2 and L2ŌĆōL3 during the 60s) should be noted because of the high acceleration of LDD. To the best of our knowledge, the present study is the first to report the high acceleration of disc degeneration during the decade of life before the prevalence of LDD at that level became greater than 50% in symptomatic patients. The aforementioned results support the fact that aging plays an important role in LDD. This LDD pattern finding may help clinicians to assess the level of patient risk according to the patientŌĆÖs age group, and may further enhance treatment-related decision-making. We also compared our symptomatic study to the 2013 asymptomatic study by Kim et al. [4] that reported the prevalence of asymptomatic LDD in patients with a mean age 46.3 years. These authors based their grading system on signal intensities. Therefore, their prevalence results tended to be close to our prevalence rates during the decade in which 50% of patients had LDD. That group also reported the acceleration of disc degeneration in the decade that preceded the decade in which the prevalence of LDD reached 50%. Compared with our results, Kim et al. [4] reported a less consistent prevalence slope for L5ŌĆōS1 LDD; nevertheless, their L5ŌĆōS1 LDD prevalence was higher than the other levels in the younger age groups. The same pattern of the progression of LDD in asymptomatic cases in the study by Kim et al. [4] and symptomatic patients in our study may support the natural program of LDD processes.
Data from the present study also showed involvement of different lumbar levels in the cases associated with the highest prevalence of LDD when single- and multiple-level degenerations were compared. The lumbar and sacral levels with the high prevalence of LDD in single-level LDD were L5ŌĆōS1. However, the L4ŌĆōL5 levels were slightly more common than the L5ŌĆōS1 levels in multilevel LDD. This observed difference between single-level and multiple-level LDD can be explained. L5ŌĆōS1 is the lumbosacral junction comprising the last levels to receive compression loads. Thus, the chance of this level being the first level to develop LDD is high. This may also be the reason why the prevalence of LDD in single-level LDD is the highest at the levels of L5ŌĆōS1 among younger aged patients. When patients become older, multilevel LDD is more common. CMDD was predominant at L4ŌĆōL5, whereas SLDD was predominant at L5ŌĆōS1. Levels L5ŌĆōS1 will less likely to combine with lumbar levels (other than L4ŌĆōL5) in CMDD types. However, L4ŌĆōL5 has two adjacent levels to combine with. This is why the chance of their combination with another level is higher compared with L5ŌĆōS1. Another reason may be anatomic protective factors, such as lumbosacral transition, iliolumbar ligament, and high-intercrestal line, because these factors were found to protect some patients from mechanical cause of disc degeneration at L5ŌĆōS1, whereas L4ŌĆōL5 is not associated with any similar protective factors [21ŌĆō24]. Studies often report their results without describing in detail the number of levels of LDD and the ratio of CMDD to SLDD. This may be one of the reasons that a variety of lumbar levels (commonly L4ŌĆōL5 or L5ŌĆōS1) for which they exhibit the highest LDD prevalence in different age groups [5,19,25,26]. If the study population predominantly consists of younger patients, LDD will be dominant at L5ŌĆōS1, and most cases will be single-level LDD. However, if most of these cases are at an advanced age, L4ŌĆōL5 will be the dominant level of LDD, and there will be a high prevalence of CMDD.
The common pattern of multiple disc degeneration was contiguous level (76.13% in the two-level degeneration group, 71.14% in the three-level group, and 70.87% in the four-level group). The degeneration usually occurs at the adjacent level, as shown in previous biomechanics and clinical studies. Natarajan and Andersson [27] conducted a biomechanical study using finite element analysis that showed the effect of degenerative disc on the sagittal angular motion at the adjacent level. Our previous study also demonstrated an adverse effect of the degenerative disc on the sagittal angular motion as evaluated by kinematic MRI [28]. The study by Cheung et al. [29] on intervertebral disc degeneration found CMDD to be far more prevalent than SLDD among studied volunteers of Southern Chinese origin with a CMDD to SLDD ratio of 7.9:2.1. In our study, the ratio of CMDD to SLDD was 7.3:2.7 for multilevel LDD in symptomatic patients. These findings seem to suggest that the CMDD to SLDD ratio may be the same in different populations. Nevertheless, these two different study populations cannot be directly compared, so this hypothesis requires further study.
The commonly observed pattern among SLDD involved the skipping of one level of nondegenerative intervertebral disc with a combination of lowermost caudad lumbar level LDD, as follows: two-level SLDD: L3ŌĆōL4 and L5ŌĆōS1, three-level SLDD: L2ŌĆōL3, L4ŌĆōL5, and L5ŌĆōS1, and four-level SLDD: L1ŌĆōL2, L3ŌĆōL4, L4ŌĆōL5, and L5ŌĆōS1. The risk factors for SLDD that were reported were male, had a history of back injury, had a documented presence of SchmorlŌĆÖs node and a bulging disc [29]. Increasing prevalence of upper and midlumbar (L1ŌĆōL2, L2ŌĆōL3, and L3ŌĆōL4) level LDD was detected in this subtype. Furthermore, preexisting injury and/or coexisting defect or pathology were more often observed in patients with LDD at higher lumbar levels [30]. Genetic and familial influences were factors reported to be significantly associated with disc degeneration, and lifetime occupations that require heavy lifting and leisure physical loading were identified as adjunct factors that increase the chance of upper lumbar LDD [25]. SLDD should be determined and the risk factors should be evaluated in patients who plan to undergo spine surgery.
The LDD findings from the present study should be used to further study the degeneration of adjacent segments to differentiate natural progression from mechanical aggravation. An adjacent segment degeneration study would also benefit from the inclusion of additional data, including the number of levels, CMDD or SLDD, and common or uncommon subtypes. Moreover, the proposed analysis must include both adjacent and all other lumbar levels to determine patterns of activity. Lastly, in contrast to our study that included mostly middle-aged patients, a future study on adjacent segment degeneration should include data that reflects a balance among different age groups.
This study was associated with limitations. First, this was a cross-sectional studyŌĆōnot a longitudinal study, which would have higher accuracy for determining patterns of LDD. Second, the population enrolled in this study was predominantly middle age, so our results may not reflect or be generalizable to other age groups of symptomatic patients. Third, there were many changing structures that influenced the pattern of disc degeneration, such as endplate changes, facet joint degeneration, facet tropism, SchmorlŌĆÖs nodes, and high-intensity zone, and these factors were not analyzed in this study. Lastly, we did not evaluate or analyze the association between MRI finding and clinical data specific to the degree of patient symptoms attributed to the lack of clinical data specific to low-back pain based on a standard scoring system. The strength of this study is that it provides baseline information from a large cohort of symptomatic patients that can be used for comparison with future cases to improve treatment planning.
This cross-sectional study used MRI to determine the prevalence of natural patterns of LDD in symptomatic middle-aged patients. LDD was more common in the lower lumbar spine, and the number of levels of LDD and the degree of LDD increased with age. The specific pattern and rate of LDD depended on the lumbar disc level and age. This LDD pattern data can be used before spinal procedures to predict the likelihood of natural LDD progression with age, and this preoperative assessment will enhance treatment planning and outcomes.
Conflict of Interest
Conflict of Interest
No potential conflict of interest relevant to this article was reported.
Acknowledgments
The authors gratefully acknowledge Miss Nhathita Panatreswas for statistical analysis.
Fig.┬Ā1
Plot showing moderate correlation between total LDD score and age (PearsonŌĆÖs correlation coefficient: 0.649). LDD, lumbar disc degeneration.
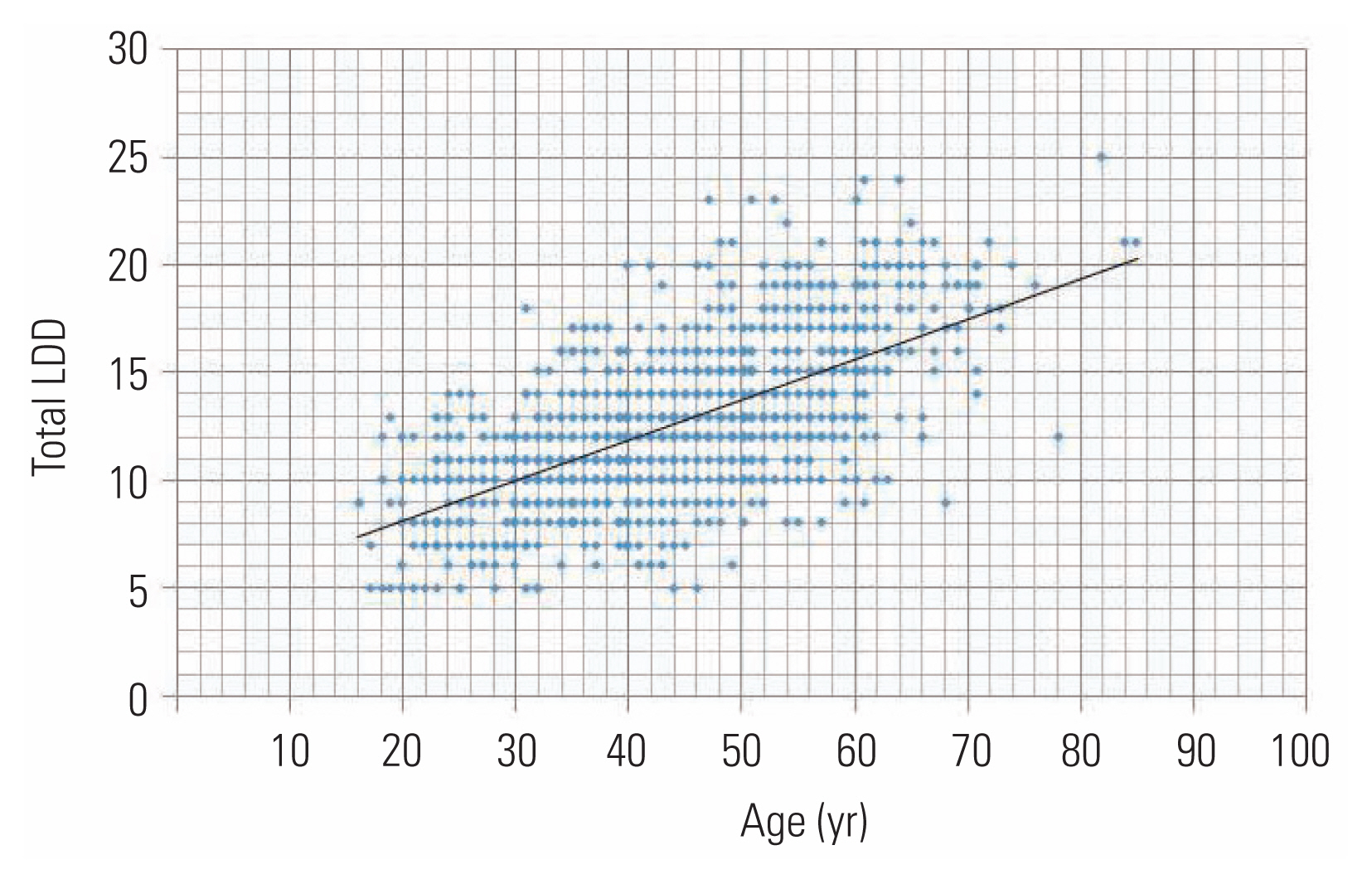
Fig.┬Ā2
Percentage of LDD compared among lumbar levels by the age by decade. LDD, lumbar disc degeneration. a)Represents the age by decade during which the percentage of LDD for that lumbar disc level became greater than 50%.

Fig.┬Ā3
Distribution of the number of levels of LDD according to the age by decade. LDD, lumbar disc degeneration.

Table┬Ā1
Disc degeneration grading system
Table┬Ā2
Distribution of the number of levels of LDD compared among different levels of lumbar intervertebral disc involvement
Table┬Ā3
Multilevel-LDD patterns compared between CMDD and SLDD
References
1. Tertti MO, Salminen JJ, Paajanen HE, Terho PH, Kormano MJ. Low-back pain and disk degeneration in children: a case-control MR imaging study. Radiology 1991 180:503ŌĆō7.


2. Jarvik JJ, Hollingworth W, Heagerty P, Haynor DR, Deyo RA. The Longitudinal Assessment of Imaging and Disability of the Back (LAIDBack) Study: baseline data. Spine (Phila Pa 1976) 2001 26:1158ŌĆō66.


3. Cheung KM, Karppinen J, Chan D, et al. Prevalence and pattern of lumbar magnetic resonance imaging changes in a population study of one thousand forty-three individuals. Spine (Phila Pa 1976) 2009 34:934ŌĆō40.


4. Kim SJ, Lee TH, Lim SM. Prevalence of disc degeneration in asymptomatic Korean subjects. Part 1: lumbar spine. J Korean Neurosurg Soc 2013 53:31ŌĆō8.




5. Takatalo J, Karppinen J, Niinimaki J, et al. Prevalence of degenerative imaging findings in lumbar magnetic resonance imaging among young adults. Spine (Phila Pa 1976) 2009 34:1716ŌĆō21.


6. MacGregor AJ, Andrew T, Sambrook PN, Spector TD. Structural, psychological, and genetic influences on low back and neck pain: a study of adult female twins. Arthritis Rheum 2004 51:160ŌĆō7.


7. Chou D, Samartzis D, Bellabarba C, et al. Degenerative magnetic resonance imaging changes in patients with chronic low back pain: a systematic review. Spine (Phila Pa 1976) 2011 36(21 Suppl): S43ŌĆō53.


8. Bae JS, Lee SH, Kim JS, Jung B, Choi G. Adjacent segment degeneration after lumbar interbody fusion with percutaneous pedicle screw fixation for adult low-grade isthmic spondylolisthesis: minimum 3 years of follow-up. Neurosurgery 2010 67:1600ŌĆō8.



9. Ishihara H, Osada R, Kanamori M, et al. Minimum 10-year follow-up study of anterior lumbar interbody fusion for isthmic spondylolisthesis. J Spinal Disord 2001 14:91ŌĆō9.


10. Xia XP, Chen HL, Cheng HB. Prevalence of adjacent segment degeneration after spine surgery: a systematic review and meta-analysis. Spine (Phila Pa 1976) 2013 38:597ŌĆō608.


11. Han Y, Sun J, Luo C, et al. Comparison of pedicle screw-based dynamic stabilization and fusion surgery in the treatment of radiographic adjacent-segment degeneration: a retrospective analysis of single L5-S1 degenerative spondylosis covering 4 years. J Neurosurg Spine 2016 25:706ŌĆō12.


12. Ciplak NM, Suzer T, Senturk S, et al. Complications of 2-level dynamic stabilization: a correlative clinical and radiological analysis at two-year follow-up on 103 patients. Turk Neurosurg 2018 28:756ŌĆō62.

13. Pan A, Hai Y, Yang J, Zhou L, Chen X, Guo H. Adjacent segment degeneration after lumbar spinal fusion compared with motion-preservation procedures: a meta-analysis. Eur Spine J 2016 25:1522ŌĆō32.



14. Eck JC, Humphreys SC, Hodges SD. Adjacent-segment degeneration after lumbar fusion: a review of clinical, biomechanical, and radiologic studies. Am J Orthop (Belle Mead NJ) 1999 28:336ŌĆō40.

15. Lund T, Oxland TR. Adjacent level disk disease: is it really a fusion disease? Orthop Clin North Am 2011 42:529ŌĆō41.


16. Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 2001 26:1873ŌĆō8.


17. Jim JJ, Noponen-Hietala N, Cheung KM, et al. The TRP2 allele of COL9A2 is an age-dependent risk factor for the development and severity of intervertebral disc degeneration. Spine (Phila Pa 1976) 2005 30:2735ŌĆō42.


18. Siemionow K, An H, Masuda K, Andersson G, Cs-Szabo G. The effects of age, sex, ethnicity, and spinal level on the rate of intervertebral disc degeneration: a review of 1712 intervertebral discs. Spine (Phila Pa 1976) 2011 36:1333ŌĆō9.



19. Waris E, Eskelin M, Hermunen H, Kiviluoto O, Paajanen H. Disc degeneration in low back pain: a 17-year follow-up study using magnetic resonance imaging. Spine (Phila Pa 1976) 2007 32:681ŌĆō4.


20. Battie MC, Videman T, Parent E. Lumbar disc degeneration: epidemiology and genetic influences. Spine (Phila Pa 1976) 2004 29:2679ŌĆō90.


21. Luoma K, Vehmas T, Raininko R, Luukkonen R, Riihimaki H. Lumbosacral transitional vertebra: relation to disc degeneration and low back pain. Spine (Phila Pa 1976) 2004 29:200ŌĆō5.


22. Aihara T, Takahashi K, Ono Y, Moriya H. Does the morphology of the iliolumbar ligament affect lumbosacral disc degeneration? Spine (Phila Pa 1976) 2002 27:1499ŌĆō503.


23. Aihara T, Takahashi K, Ogasawara A, Itadera E, Ono Y, Moriya H. Intervertebral disc degeneration associated with lumbosacral transitional vertebrae: a clinical and anatomical study. J Bone Joint Surg Br 2005 87:687ŌĆō91.


24. Quinnell RC, Stockdale HR. The use of in vivo lumbar discography to assess the clinical significance of the position of the intercrestal line. Spine (Phila Pa 1976) 1983 8:305ŌĆō7.


25. Battie MC, Videman T, Gibbons LE, Fisher LD, Manninen H, Gill K. 1995 Volvo Award in clinical sciences: determinants of lumbar disc degeneration: a study relating lifetime exposures and magnetic resonance imaging findings in identical twins. Spine (Phila Pa 1976) 1995 20:2601ŌĆō12.


26. Videman T, Battie MC, Gill K, Manninen H, Gibbons LE, Fisher LD. Magnetic resonance imaging findings and their relationships in the thoracic and lumbar spine: insights into the etiopathogenesis of spinal degeneration. Spine (Phila Pa 1976) 1995 20:928ŌĆō35.


27. Natarajan RN, Andersson GB. Lumbar disc degeneration is an equally important risk factor as lumbar fusion for causing adjacent segment disc disease. J Orthop Res 2017 35:123ŌĆō30.


28. Kong MH, Morishita Y, He W, et al. Lumbar segmental mobility according to the grade of the disc, the facet joint, the muscle, and the ligament pathology by using kinetic magnetic resonance imaging. Spine (Phila Pa 1976) 2009 34:2537ŌĆō44.









